Vitiligo/ Leucoderma Treatment
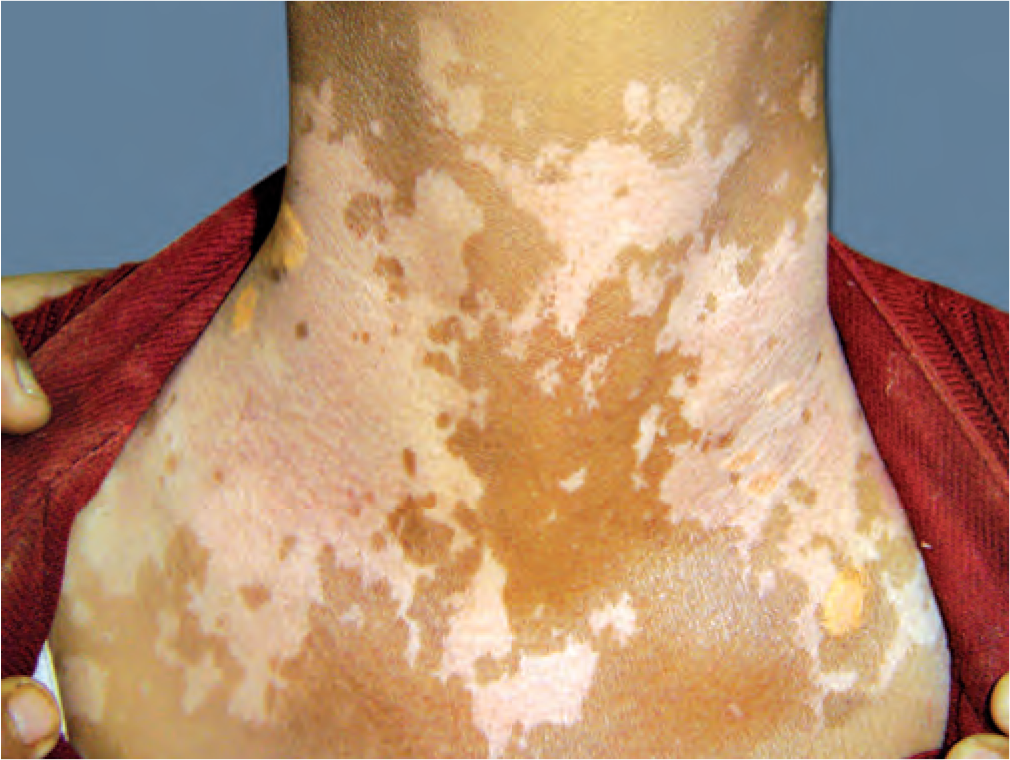
Vitiligo also known as Leucoderma or White Patches disease/white spots disease is a common depigmentation disorder, causing the skin, of the body, to go through de-pigmentation resulting in white patches or white spots that affects about 1% of the world population. On the dark skin of the body and face, these de-pigmentation patches or white spots resulting, from vitiligo, have a very striking and disfiguring effect causing severe psychological problems.
Though the exact aetiology or reason for Vitiligo or white patches disease/white spots disease to affect the body and face still remains unclear the most commonly accepted and best of all the hypothesis, clinic and hospital doctors believe, is that it’s an autoimmune disorder, in which the body’s immune system sees the cells with pigmentation, in the skin, as foreign body, and attacks them.
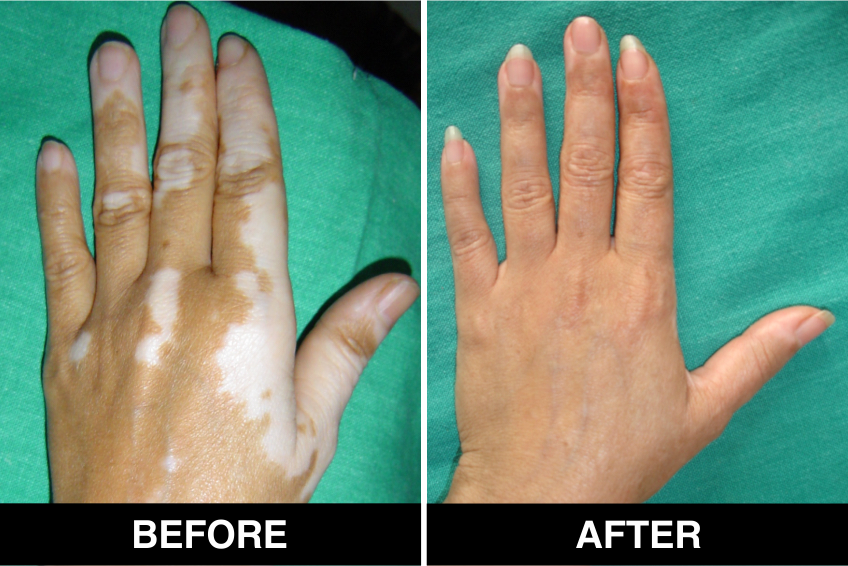
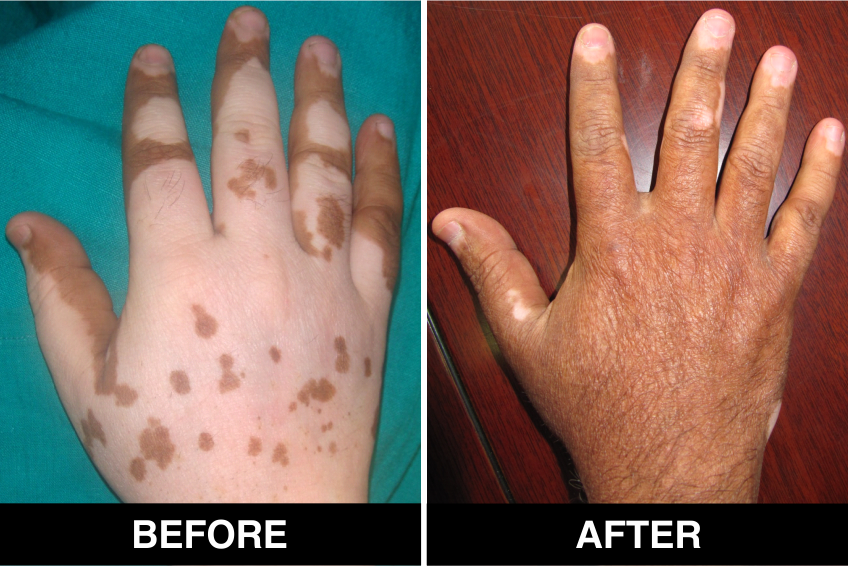
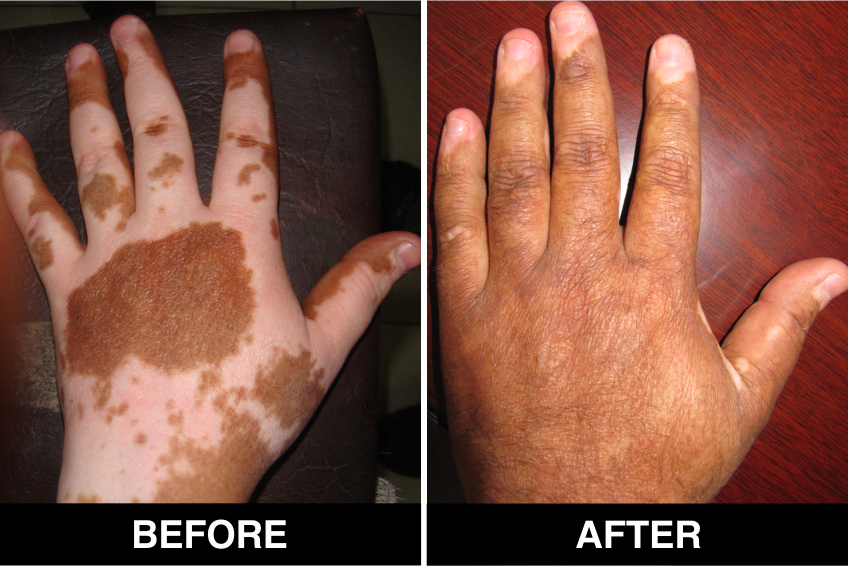
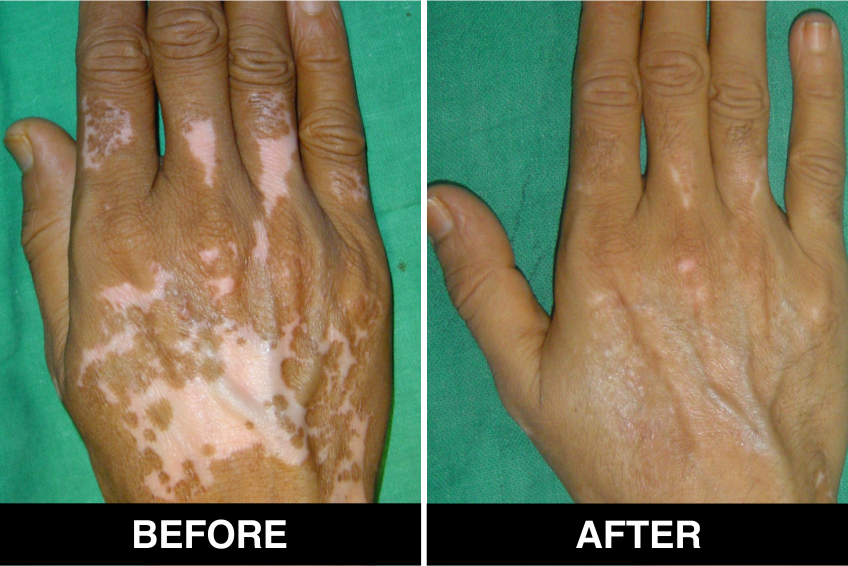
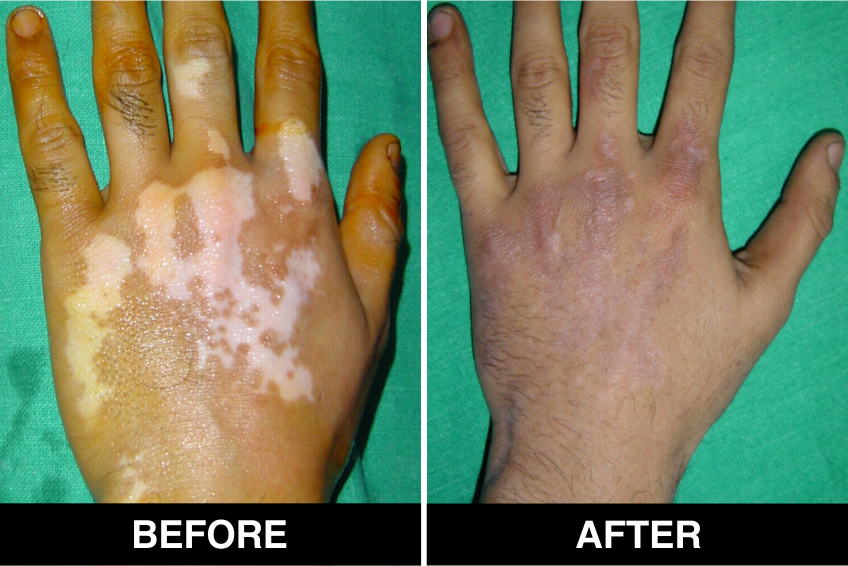
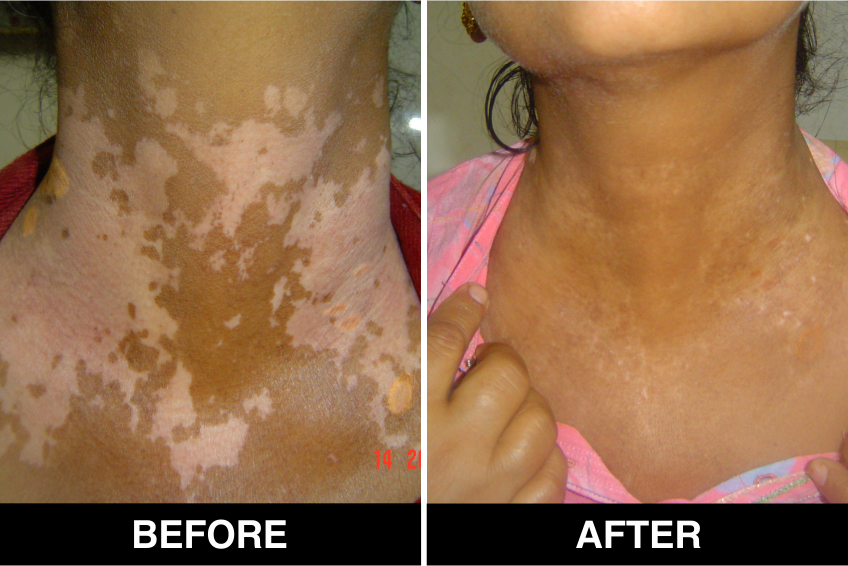
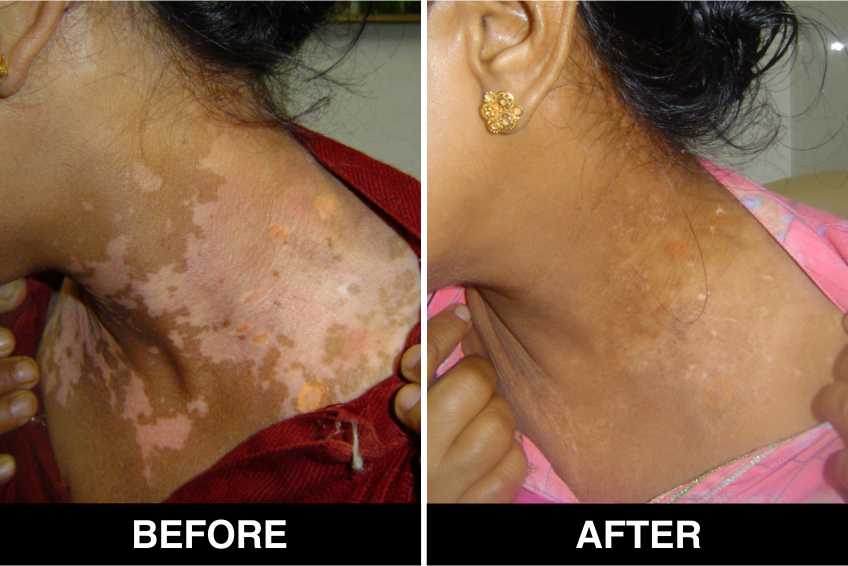
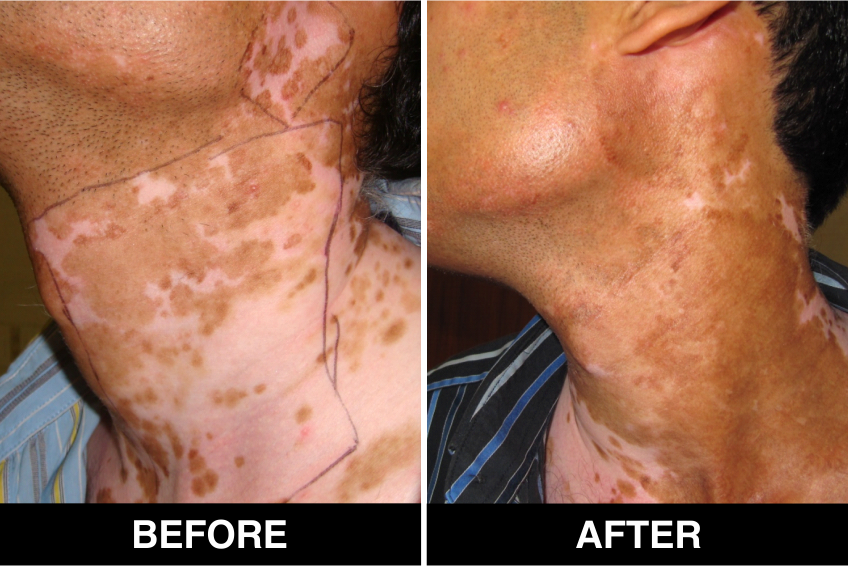
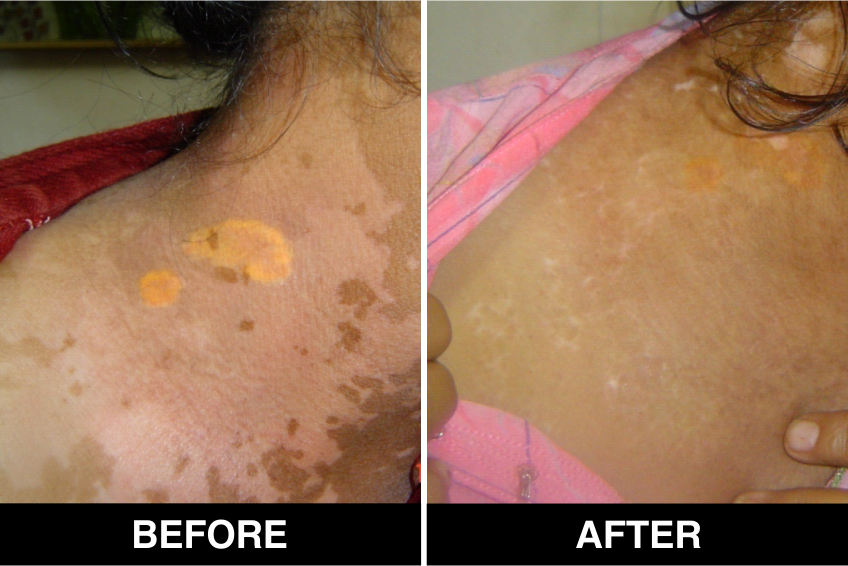
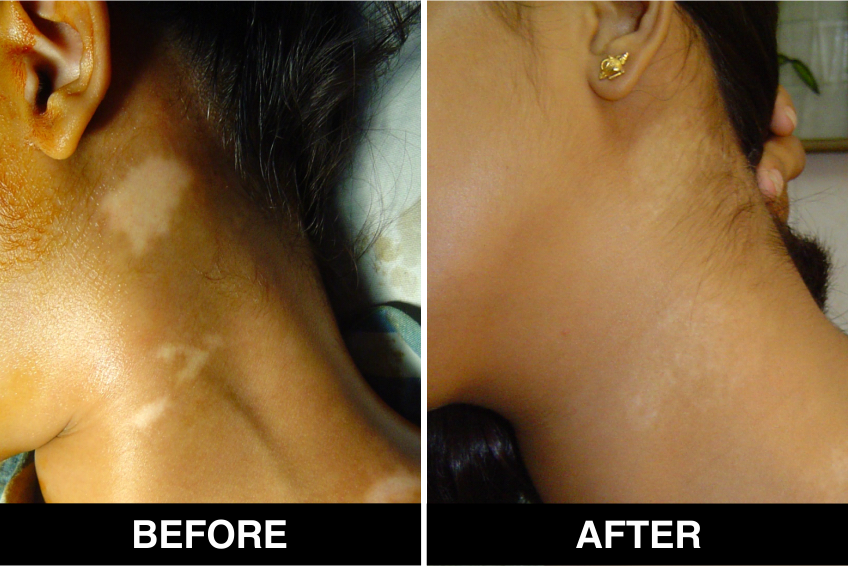
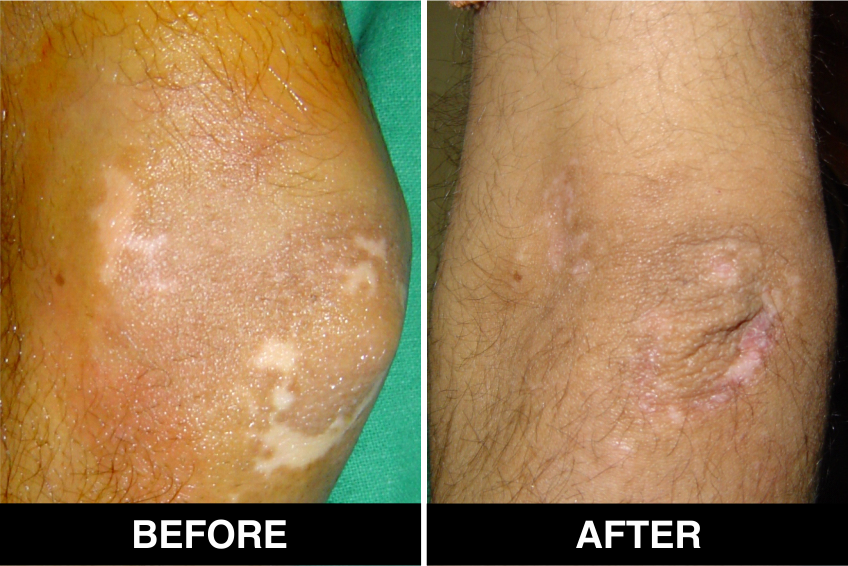
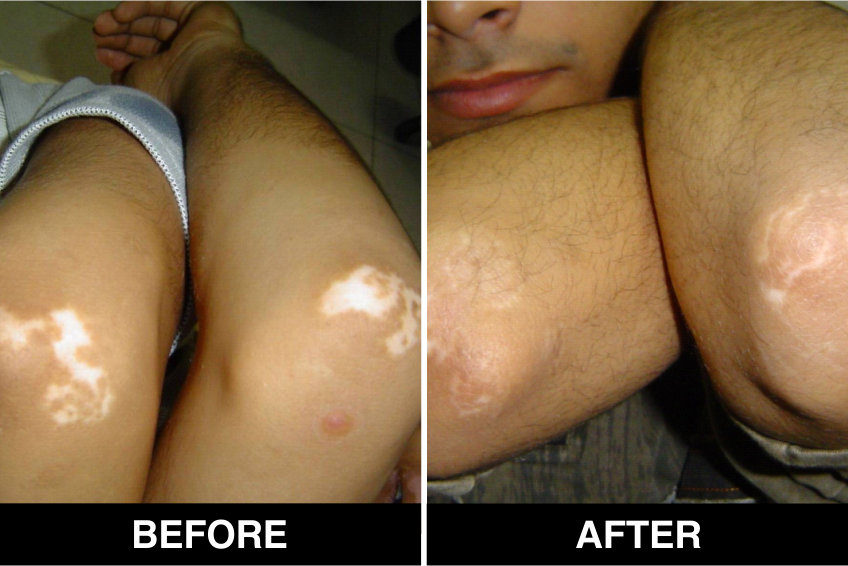
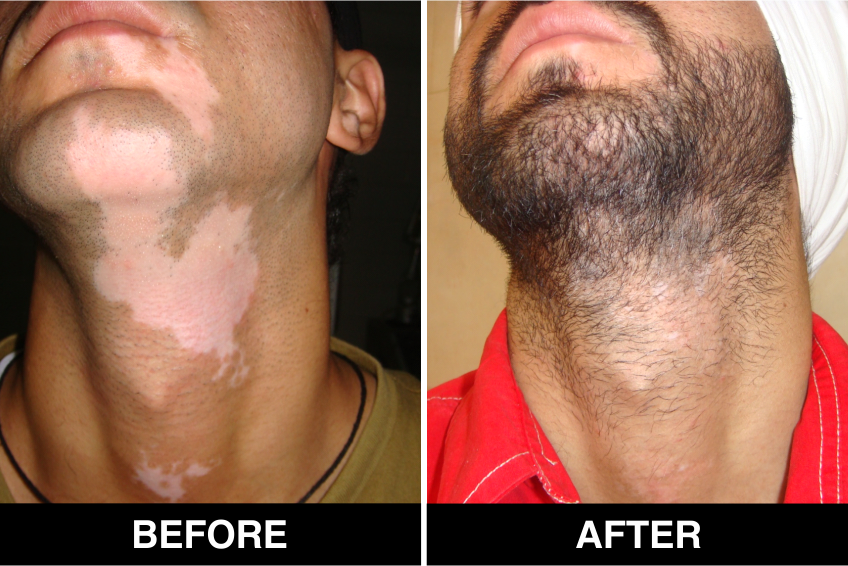
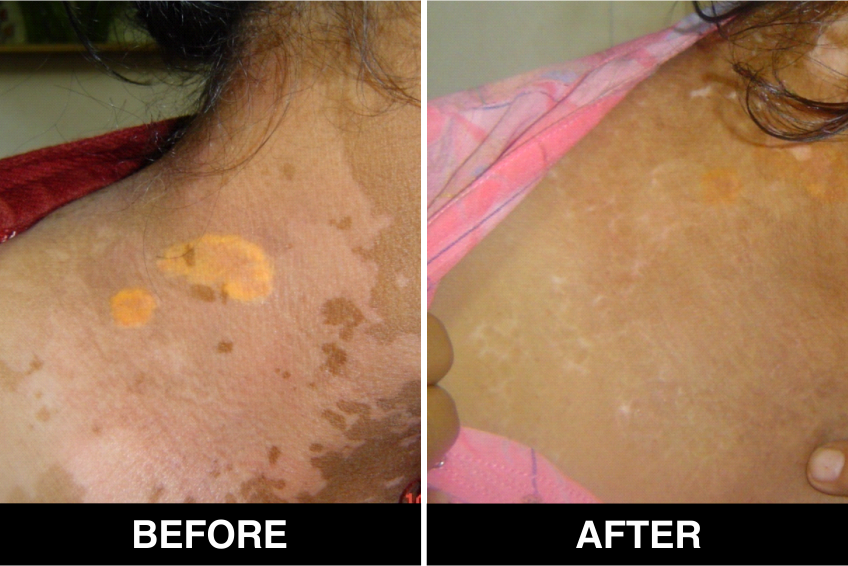
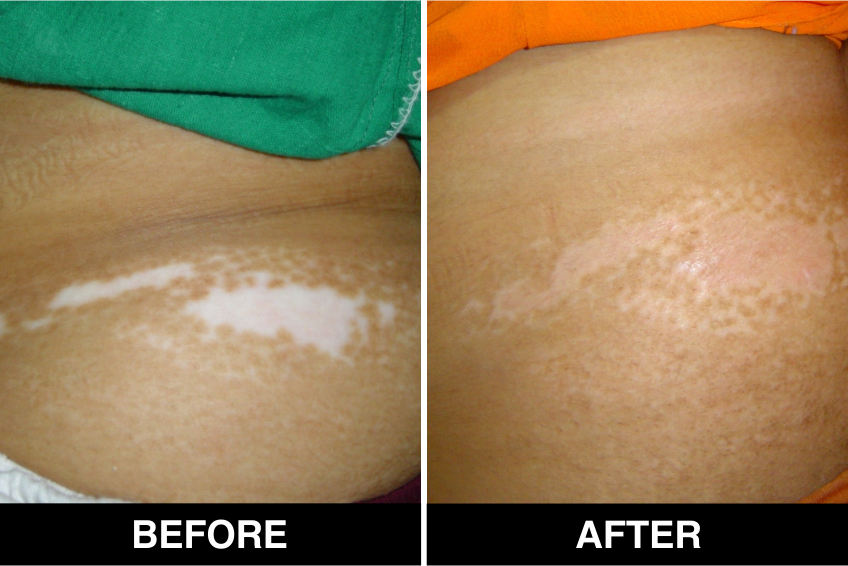
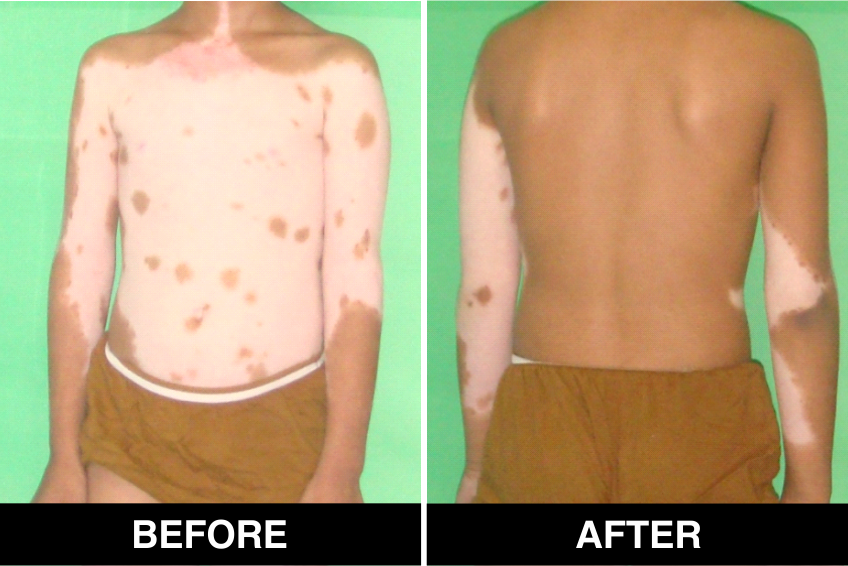
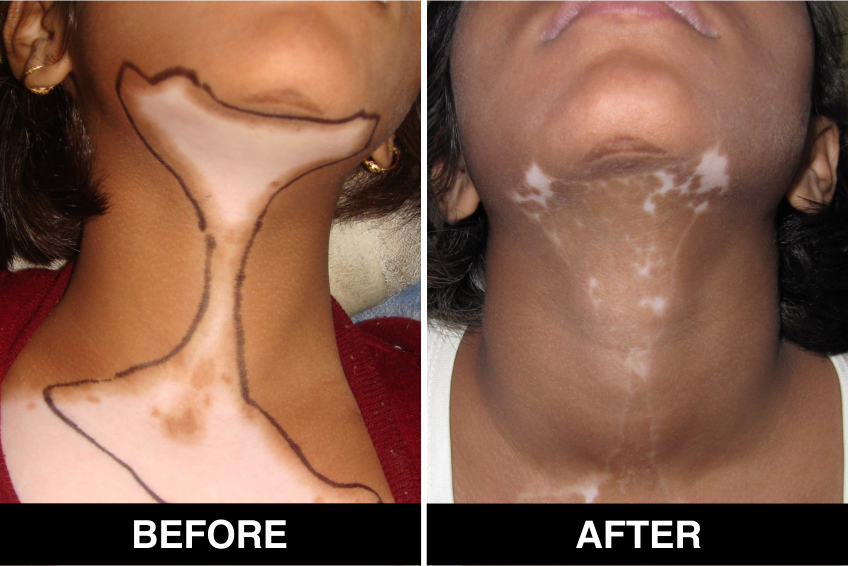
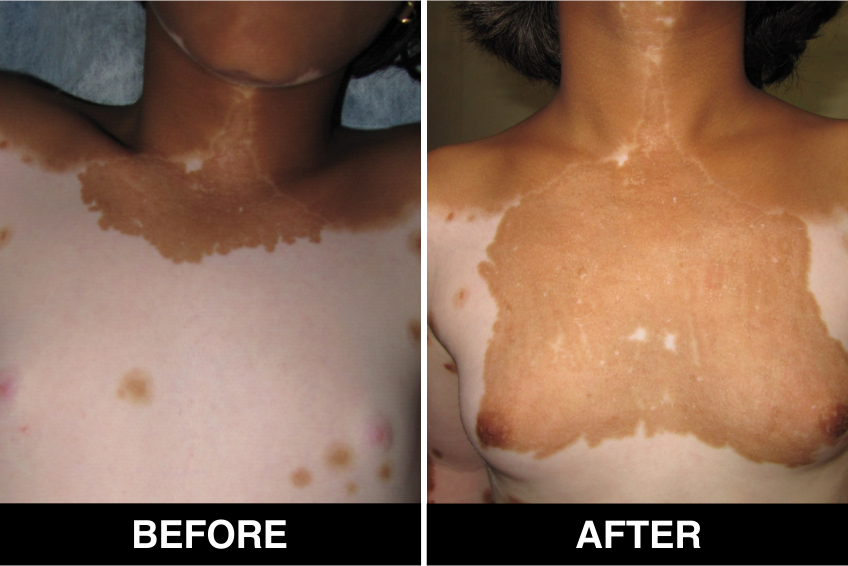
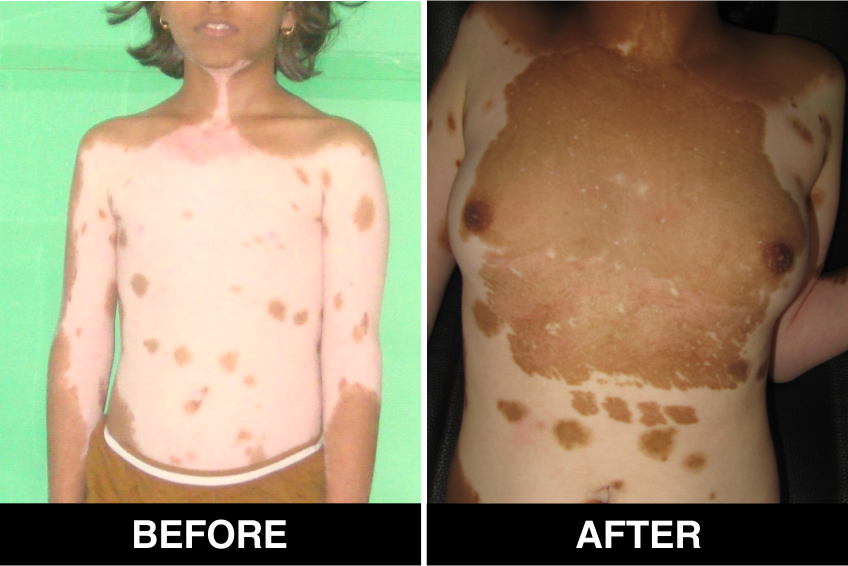
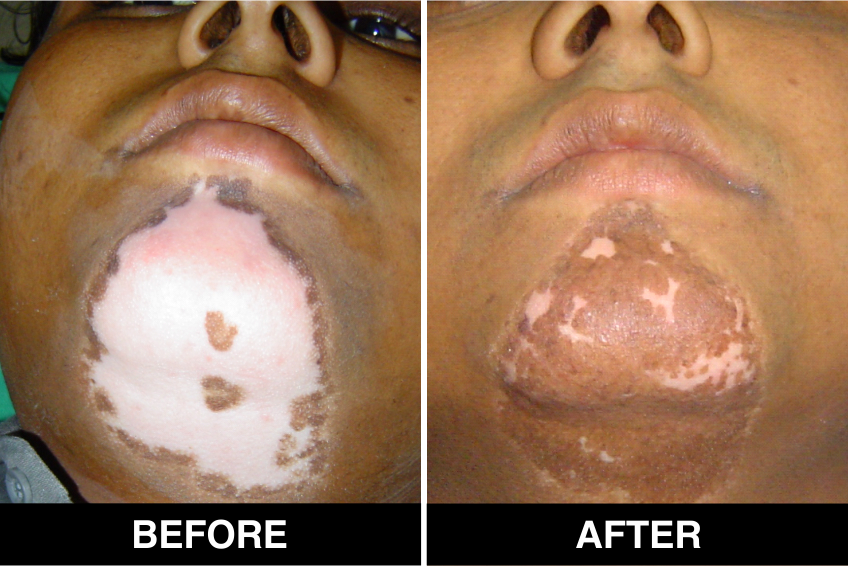
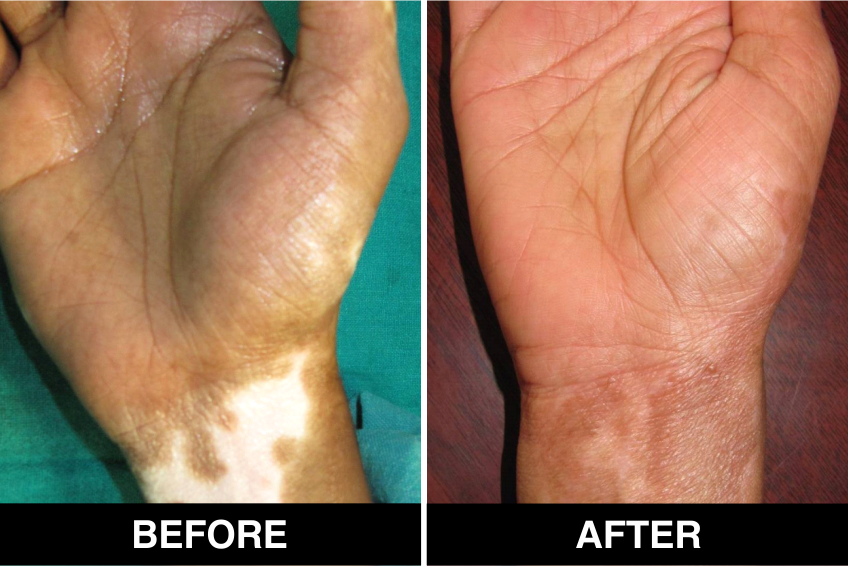
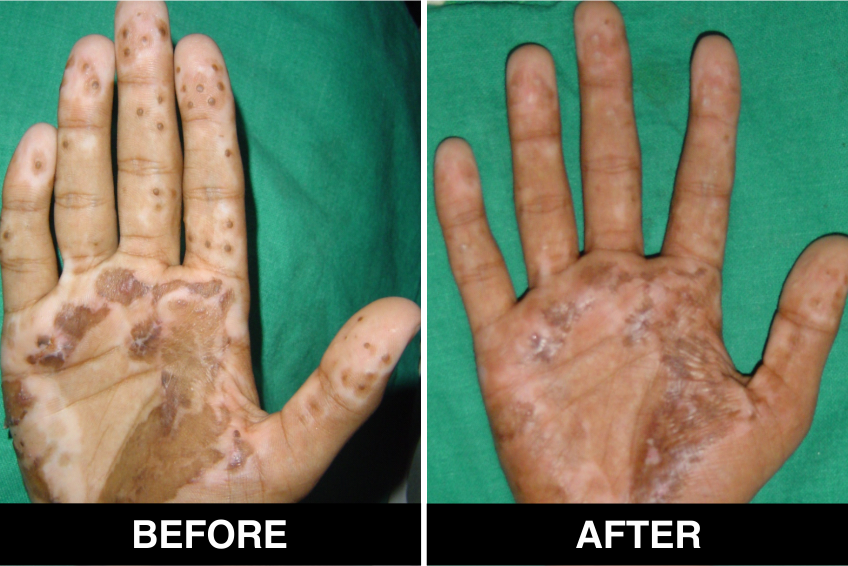
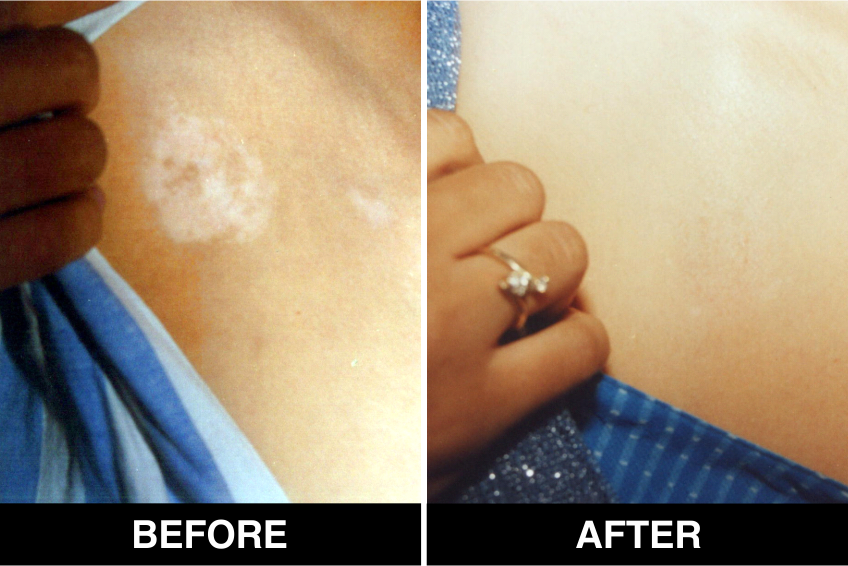
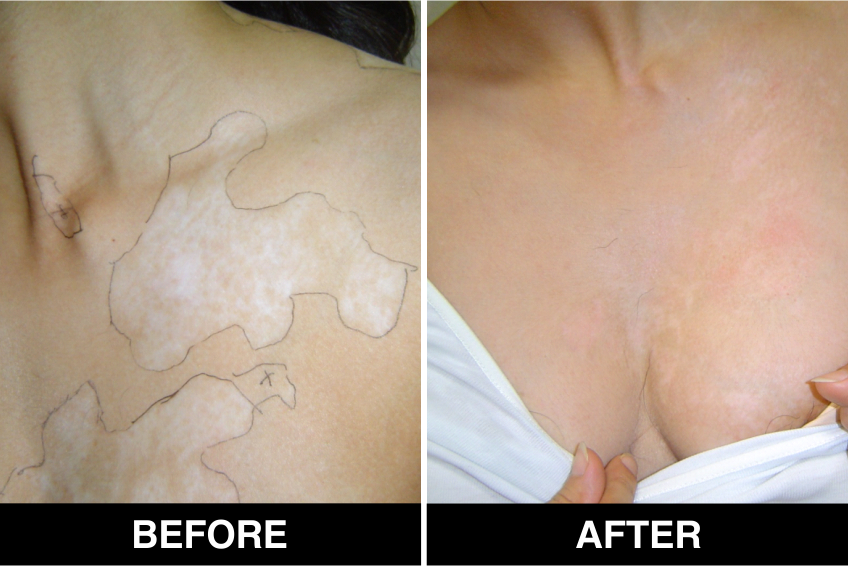
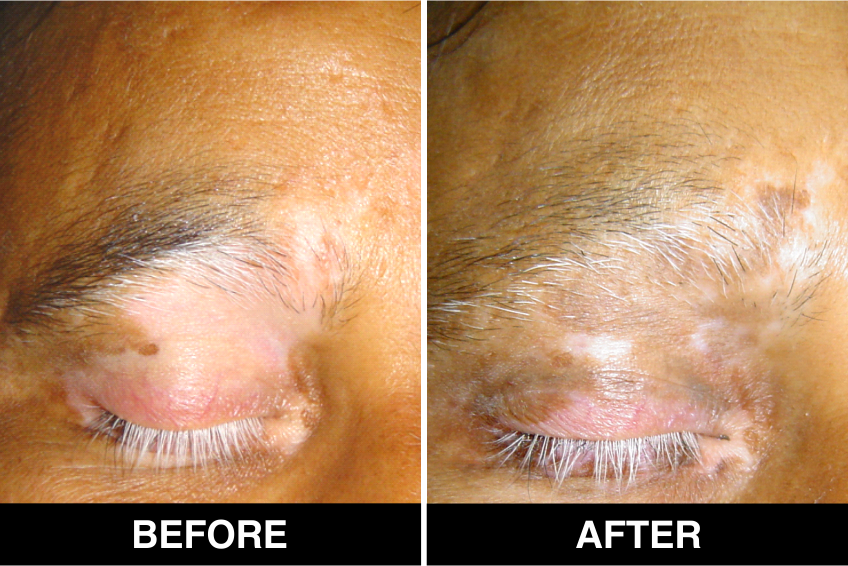
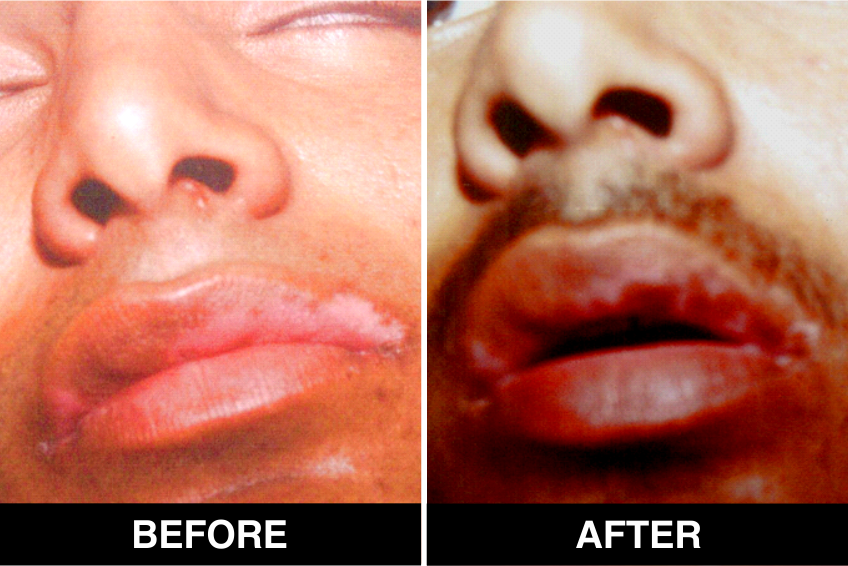
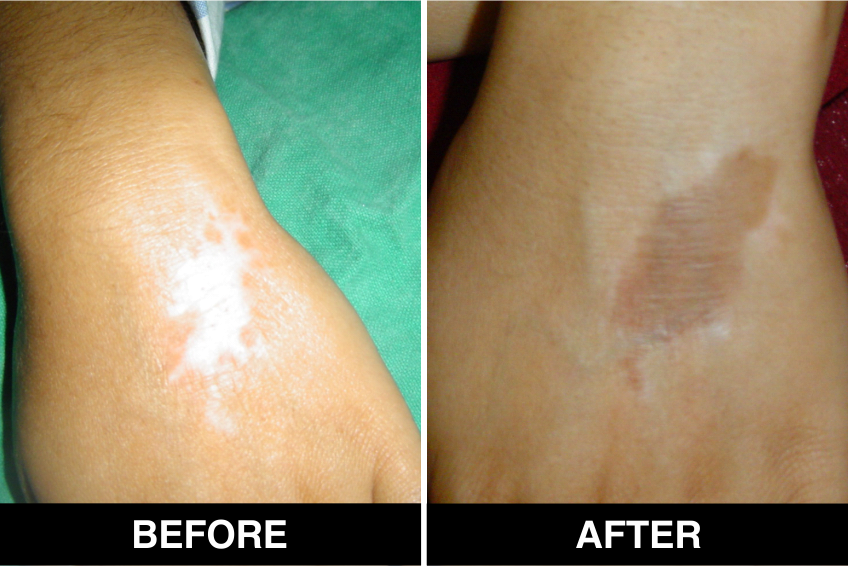
Vitiligo / White Patches Treatments
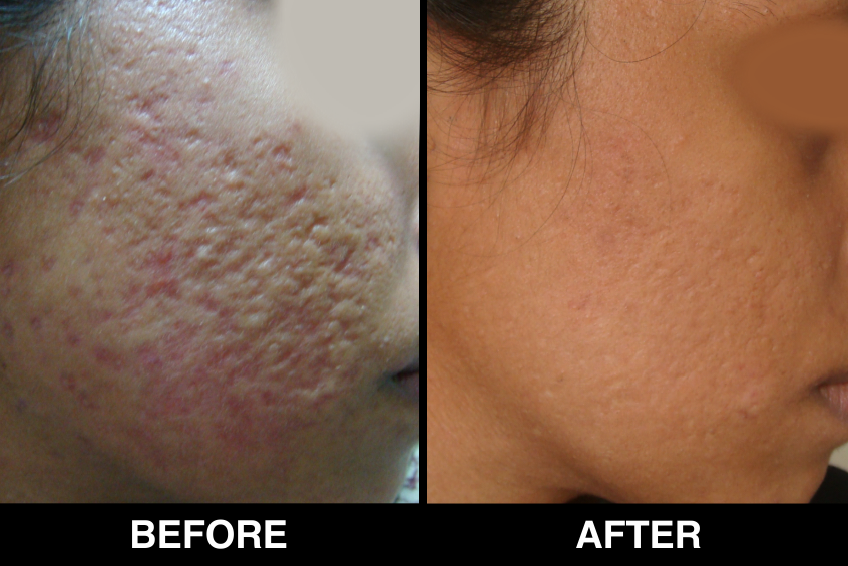
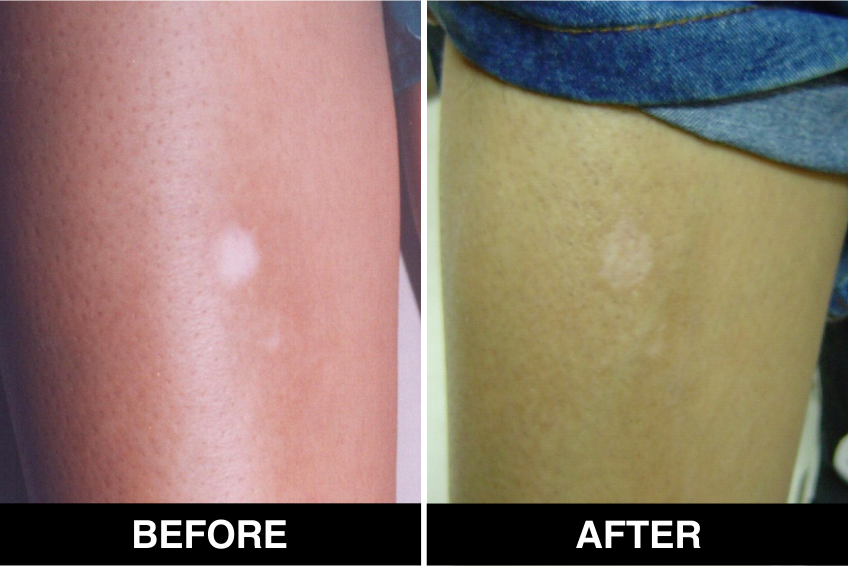
Vitiligo Treatment or White Patches Treatment is based on improving your skin’s appearance by restoring its colour. Re-pigmentation treatment is most successful on face and trunk; hands, feet and areas with white hair respond poorly. Compared to long standing patches, new ones are more likely to respond to medical therapy.
The Treatment is Classified into
- Medical treatment
- Surgical treatment
- De-pigmentation
Medical Procedures & Treatments
Medicines Applied to the Skin, such as:
- Corticosteroid
- Immunomodulator
- Oral Medical treatment
Phototherapy NBUVB Full Body:
 One of the best medical procedure or treatment, performed in approved clinics, skin centers and hospitals with renowned doctors to handle vitiligo patients in delhi, in which your body’s skin covered by white patches or white spots disease, is exposed to ultraviolet A (UVA) or ultraviolet B (UVB) light from a special lamp in full body chambers.
One of the best medical procedure or treatment, performed in approved clinics, skin centers and hospitals with renowned doctors to handle vitiligo patients in delhi, in which your body’s skin covered by white patches or white spots disease, is exposed to ultraviolet A (UVA) or ultraviolet B (UVB) light from a special lamp in full body chambers. Excimer (Targeted Phototherapy):
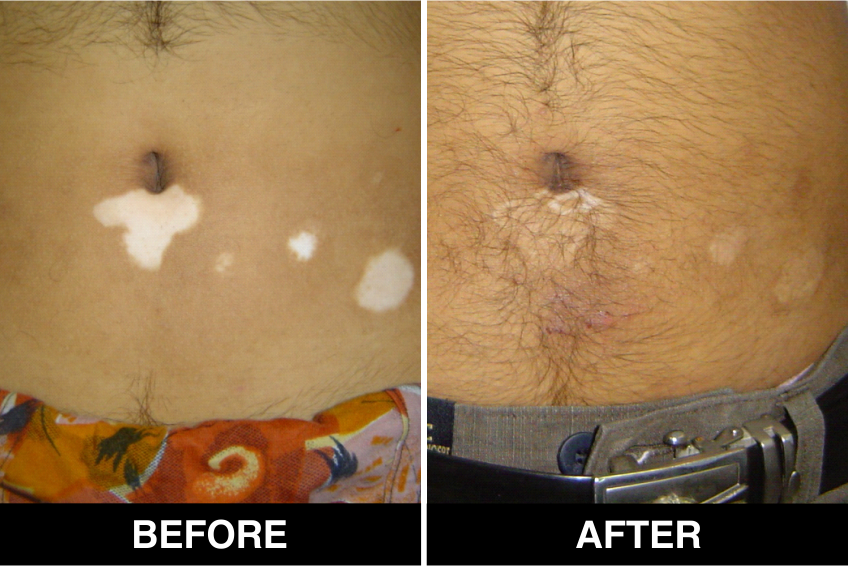
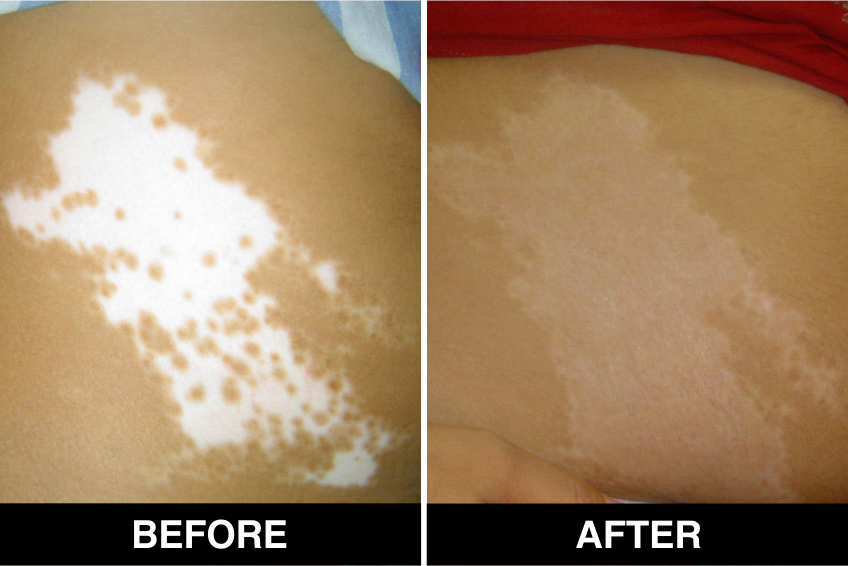
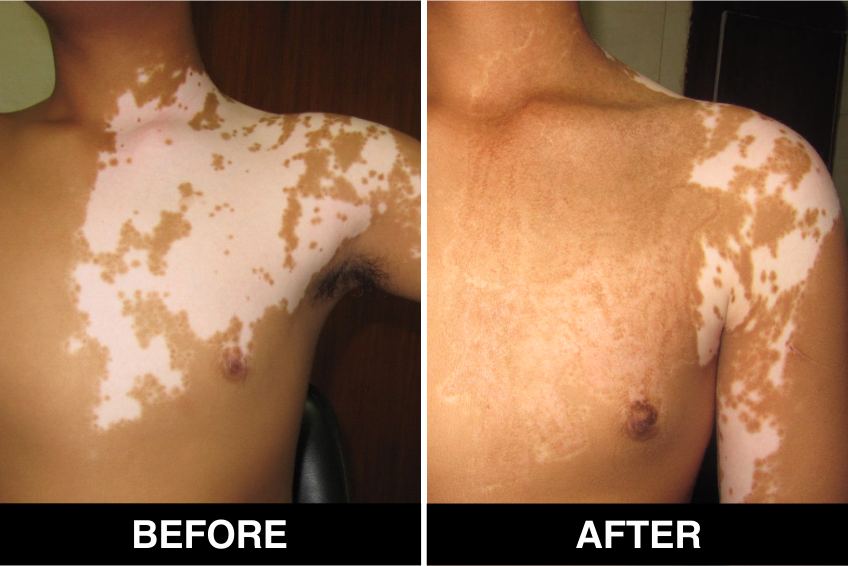
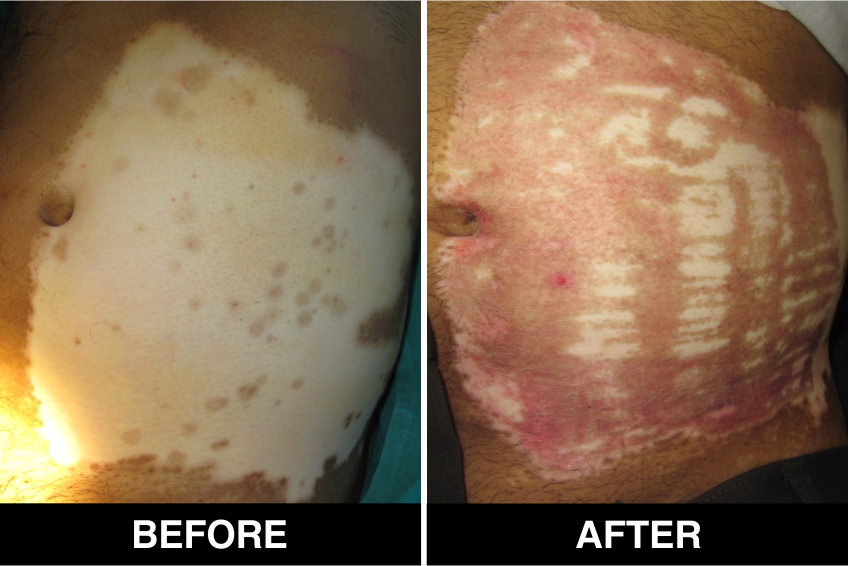
Surgical Procedures & Treatments:
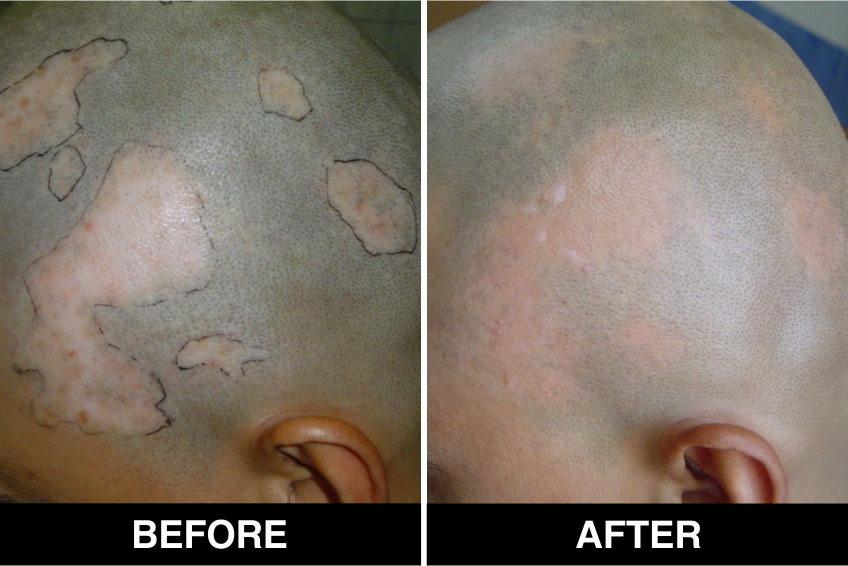
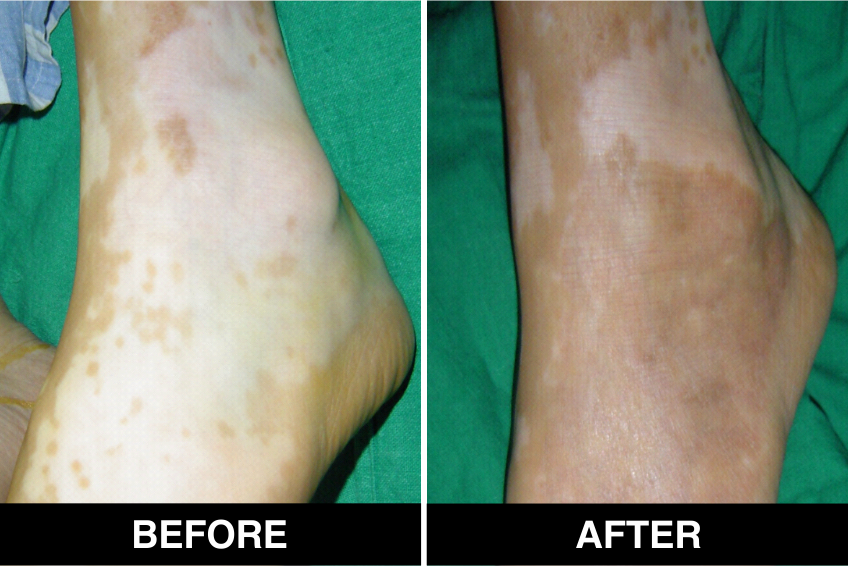
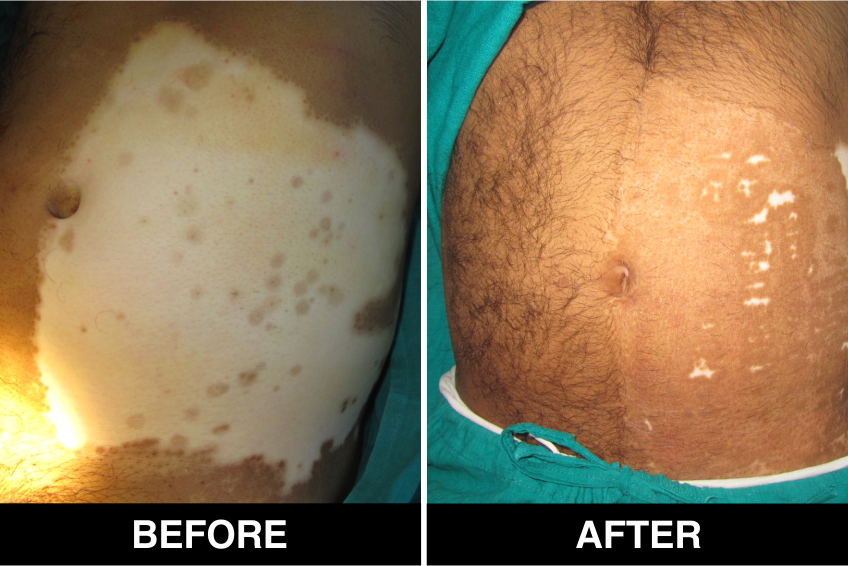
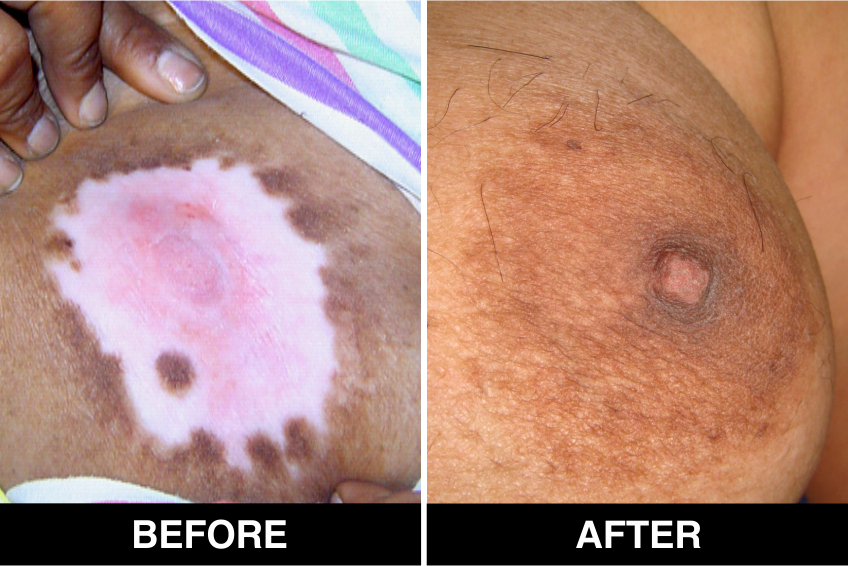
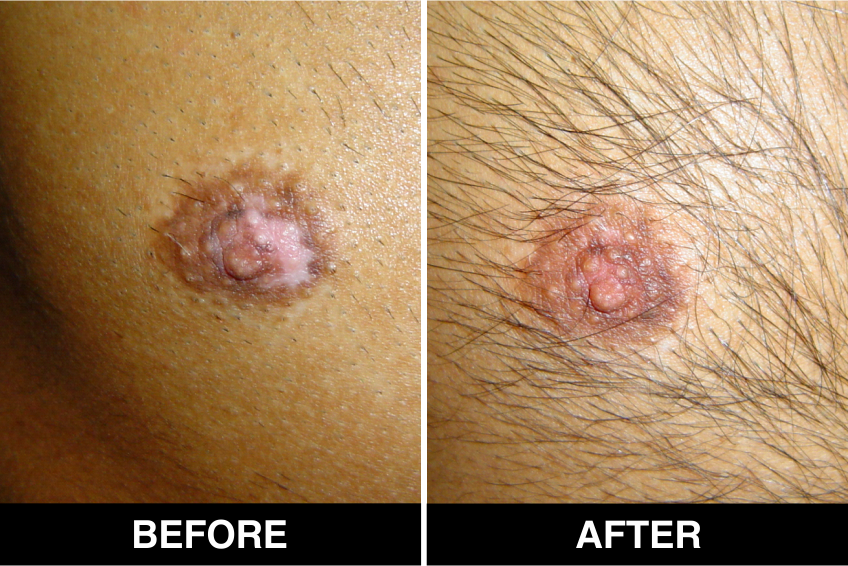
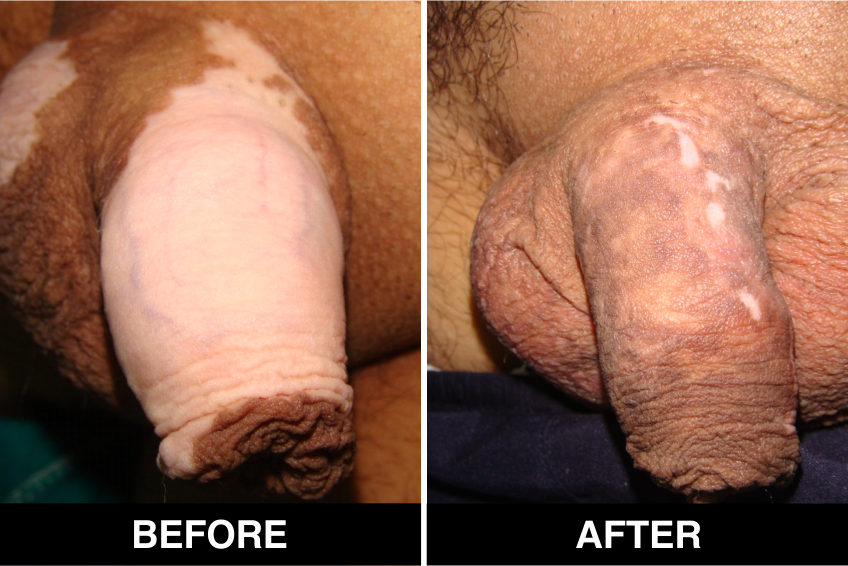
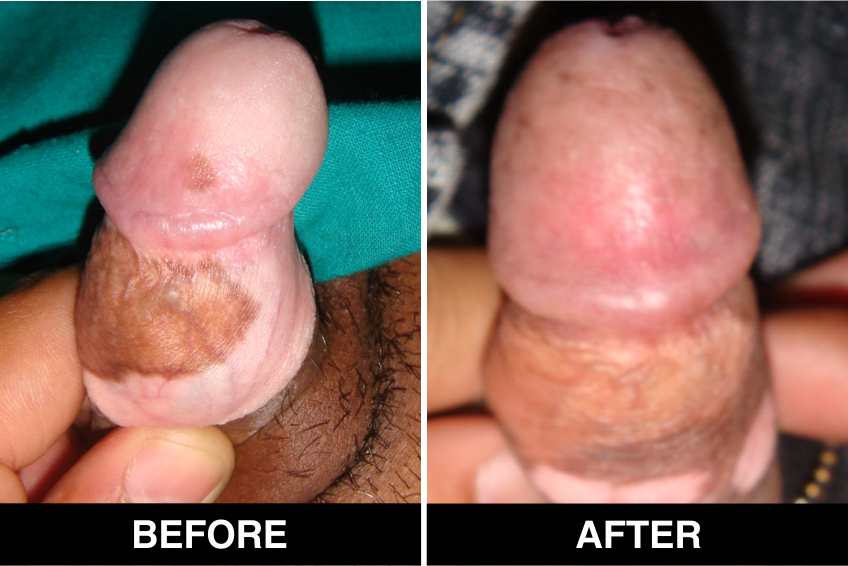
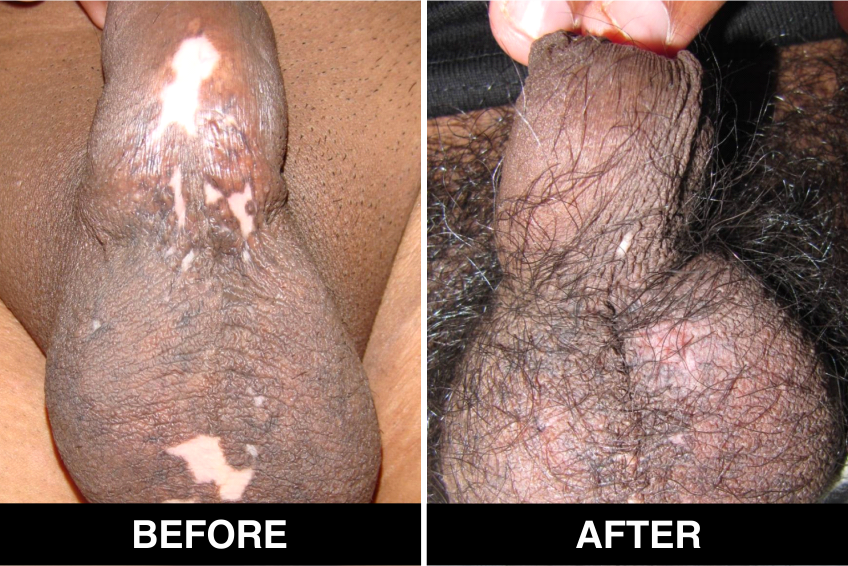
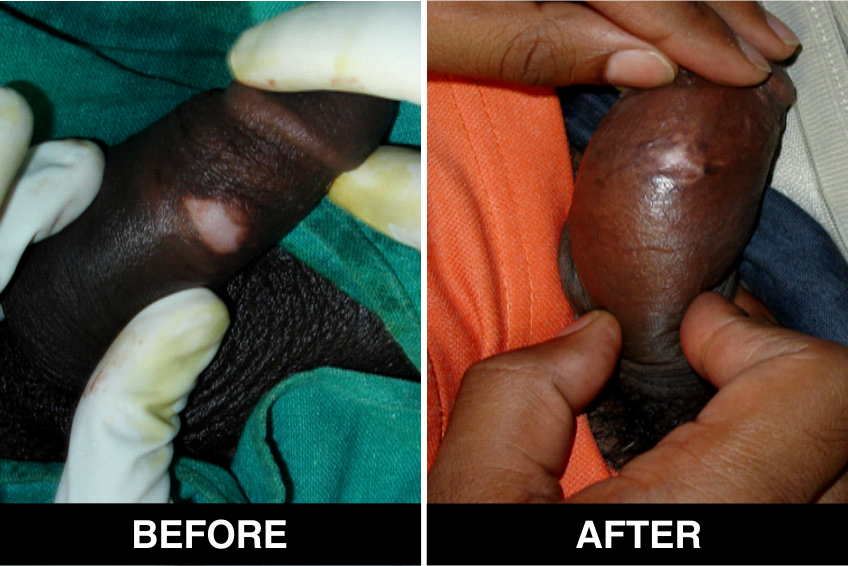
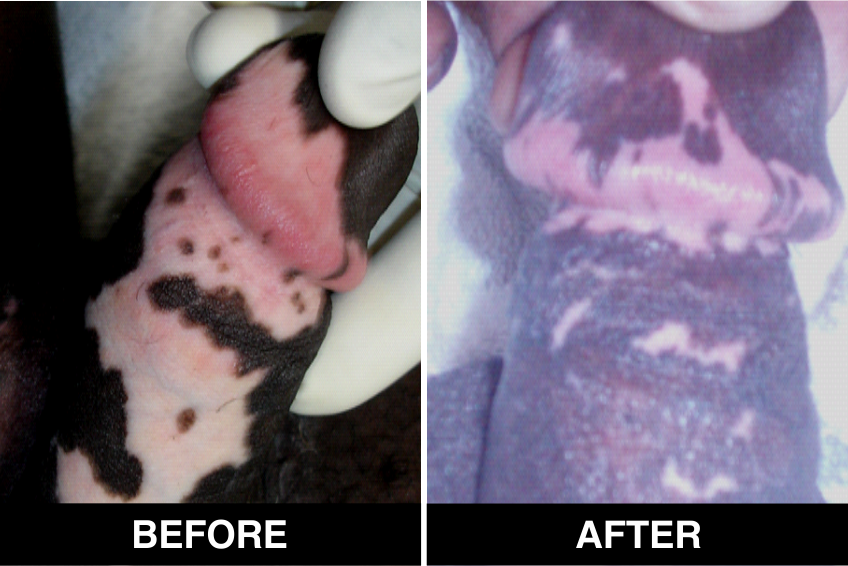
Surgical Treatment – Normal skin, from the patient’s body, is used as donor tissue and then grafts are surgically transplanted, by the doctors, in Delhi, on areas with white patches or white spots for vitiligo disease treatment. The new skin grafts start producing pigmentation on those spots. Patients, who are candidates for this treatment must have stable Vitiligo disease, or Vitiligo that has not changed for at least one year. The criteria of stability is taken as (a) no new vitiligo affected white patches or white spots on the body, (b) no extension of existing vitiligo affected White patches or white spots and (c) no loss of vitiligo affected pigmentation for at least 1 year.
This is considered to be the best course of treatment given to patients with limited areas of Vitiligo or white spots affecting their body and also in those with more extensive disease. This treatment is also performed in certain approved clinics, hospitals and skin centers in Delhi under supervision of best doctors, best skilled at treatment of the disease on the patient’s body and face covered with patches and areas of de-pigmentation.
Melanocyte Cell Transplantation – Doctors, in Delhi, treating vitiligo takes a skin graft from the patient’s own thigh, this skin, is then treated with an enzyme known as trypsin which separates all the layers of the skin and thus Melanocytes and Keratinocytes are concentrated. The skin, affected by vitiligo or white patches/ white spots disease, is then removed with the use of diamond burs or Lasers and the cells are transplanted in the affected areas of the body.
The best advantage of this treatment is that cell culture is not needed and that skin harvesting from the donor area, preparation of cell separation and application of Melanocytes can all be undertaken in a single 3-h procedure, all performed by the doctor deemed fit with the best of his/her abilities clinically, for treatment of Vitiligo or white patches disease or white spots disease on the patient’s body and face, covered with patches and areas of de-pigmentation, in certain approved clinics, hospitals and skin centers by doctors in Delhi.
(Read more under Melanocyte cell transplantation on the home page)
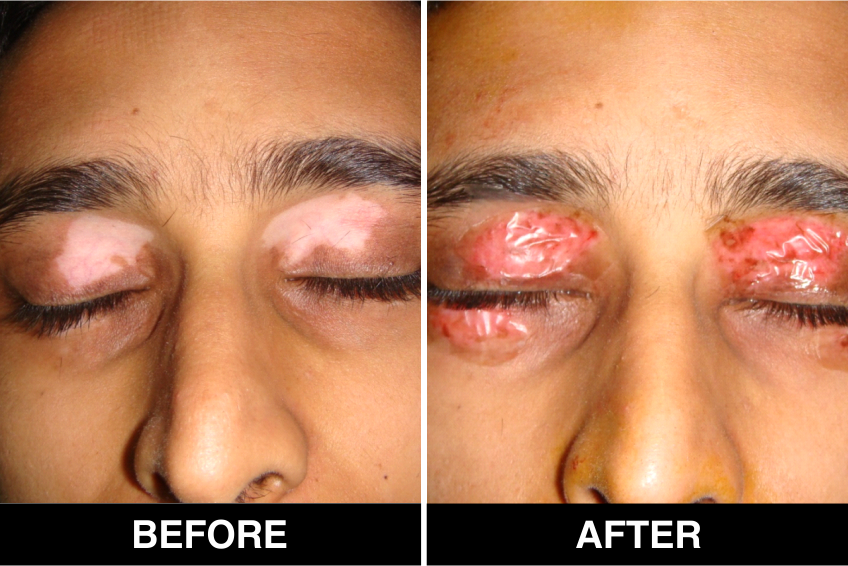
Blister Grafting – In this treatment of Vitiligo or white spots disease in Delhi, doctors create blisters are created on your skin having pigmentation, like the body and face, primarily by using suction, operated by a doctor in a clinic or hospital. The blisters are then cut out and transplanted to a skin area, not affected by pigmentation where a blister of equal size has been created and removed by doctors in Delhi.
(More Details Under section of Case study)
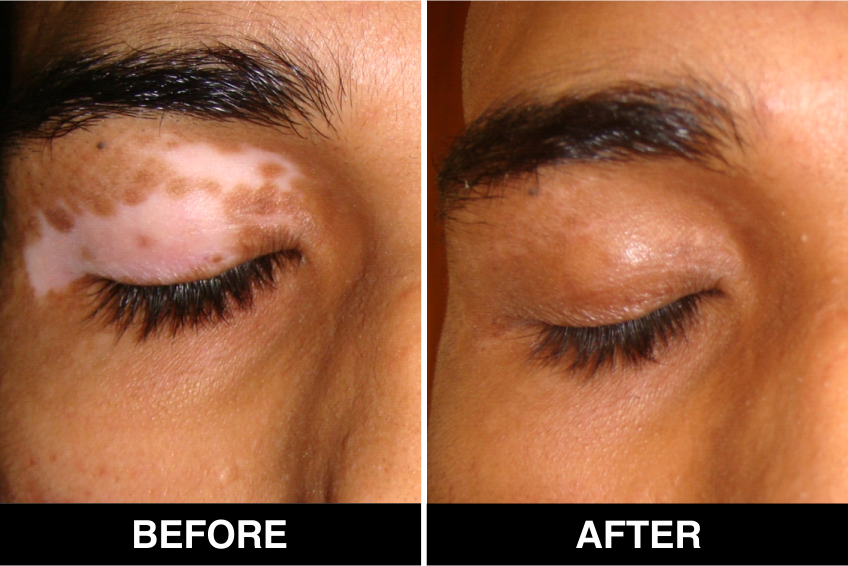
Punch Grafting – In Delhi, doctors explain punch grafting as the least expensive and one of the best of all the skin grafting treatments in Vitiligo or white spots disease, performed in certain approved clinics, hospitals and skin centers, in Delhi, under supervision of best doctors, best skilled at treating the disease, involves the transfer of circular pieces or punches of skin tissue from the donor area into similar shaped pits that are made on the recipient affected area of body or face, covered with patches or spots and areas of de-pigmentation. The size of these punches can range from 1 mm to 2 mm and they are spaced 5-10 mm apart on the recipient skin.
De-pigmentation – De-pigmentation, in certain approved clinics, hospitals and skin centers, in Delhi, under supervision of best doctors, best skilled at treating the disease, involves fading the rest of the skin on your body, or face, to match the areas with white patches or white spots. Vitiligo or white spots disease on more than 50 percent of a patient’s body, depigmentation is the best treatment option for white spots disease.
In this procedure, the clinics drug monobenzone is applied twice a day to the pigmentation areas of your skin, including face, hands and feet, until they match the areas without pigmentation. Some patients, who are resistant to depigmentation with clinic drug monobenzone will need Q Switch NDYAG Laser, available in approved clinics, skin centers or hospitals, to destroy the cells with pigmentation caused by vitiligo giving patients the best possible results by doctors in delhi.
Color (Camouflage) – Camouflage used to treat vitiligo or white spots disease can be best classified into two- temporary and permanent treatments. In delhi, doctors use temporary colouring as the clinic method which intends to blend the
White Patches or spots caused by vitiligo with the rest of the body’s skin colour. The method is done in approved clinics, skin centers or hospitals in Delhi, by the best doctors available, with coloured creams on the skin affected with patches and pigmentation. Those creams will have the same shade as that of the natural skin. These creams makes the patches or spots, due to vitiligo, less noticeable. It is advised to get this treatment in an approved clinic, hospital or skin centers under supervision of best doctors, best skilled at treating the disease, in Delhi.
Tattooing (Permanent Coloring) – In Delhi, Tattooing is injecting artificial pigment into the areas with pigmentation or white patches/spots caused by Vitiligo. After selecting the pigment shade which matches the surrounding skin colour of the body, the pigment granules are implanted into the patches with pigmentation either with a manual or electrical driven needles in the clinic. Though the pigmentation patches resembles the surrounding normal skin, it may permanently fade. Hence, tattooing is not the best of solutions unless the patch is inoperable and performed in a clinic, hospital or skin centers in Delhi under supervision of best doctors, best skilled for treatment of the disease.
Salient Features of Vitiligo Treatment by Skin Laser Centre:
- Complete Treatment under the supervision of a Board certified MD Dermatologist
- Complete open and honest discussions about treatment, chances of recovery, positive and negative effects of the treatment
- Use of Latest Technology including Full Body UV chambers, Excimer, Cell transplantation .. all under one roof
- Vitiligo Patient Testimonials
Vitiligo FAQ’s
Vitiligo can worsen with stress, also in some cases use of plastic or rubber chappals can trigger Chemical Leucoderma, In india the use of bindis, kumkum, hair dyes containing PPD can also trigger Vitiligo
Vitiligo occurs at times over site of injury so patients should be aware of this,
FOOD HAS NO ROLE
Dont worry ,there are no risk of skin cancer because of Vitiligo.
Vitiligo is a unpredictable disease , it may stable for years or it can spread ,
Factors like Strong family history, very early age of onset, Association of diseases like thyroid, patches having white hair, occurance over lip tip area ie fingers, toes lips point to a more difficult disease
One of the common symptoms of Vitiligo is that the skin will have white patches in the affected areas. The white patches can occur on any part of the body ie hands, legs, lips, mouth and armsarmpit, groin, eyes, nostrils, navel and genitals.
In focal pattern this white patches will be seen only in some few areas and in segmental pattern this white patches will be seen in one side of the body and in bilateral pattern this white patches will be seen different parts of the body. Sometimes vitiligo may be associated with white hair (Leukotrichia)
These two conditions are entirely different from each other. Leprosy is an infection caused by a bacteria in which patient develops light colored patches with loss of sensation and loss of hair
Vitiligo on the other hand occurs because of loss of melanin pigment from the skin, there is no loss of sensation, and besides cosmetic issue its not a disease as such
About 1 percent of the world's population, (50 million people), have vitiligo. In India more than 1 million cases of Vitiligo are reported per year. It is suspected that some countries may have higher incidents of vitiligo, for various genetic and societal reasons.
Vitiligo is not contagious in any way , it doesnt spread by contact touching, sharing food or clothes The precise cause of Vitiligo is not well-understood, though it seems to be the result of a combination of genetic, immunologic, biochemical and neurogenic factors. It is often, though not always, seen in families.
Book An Appointment