Melanocyte Cell Transplantation
Introduction
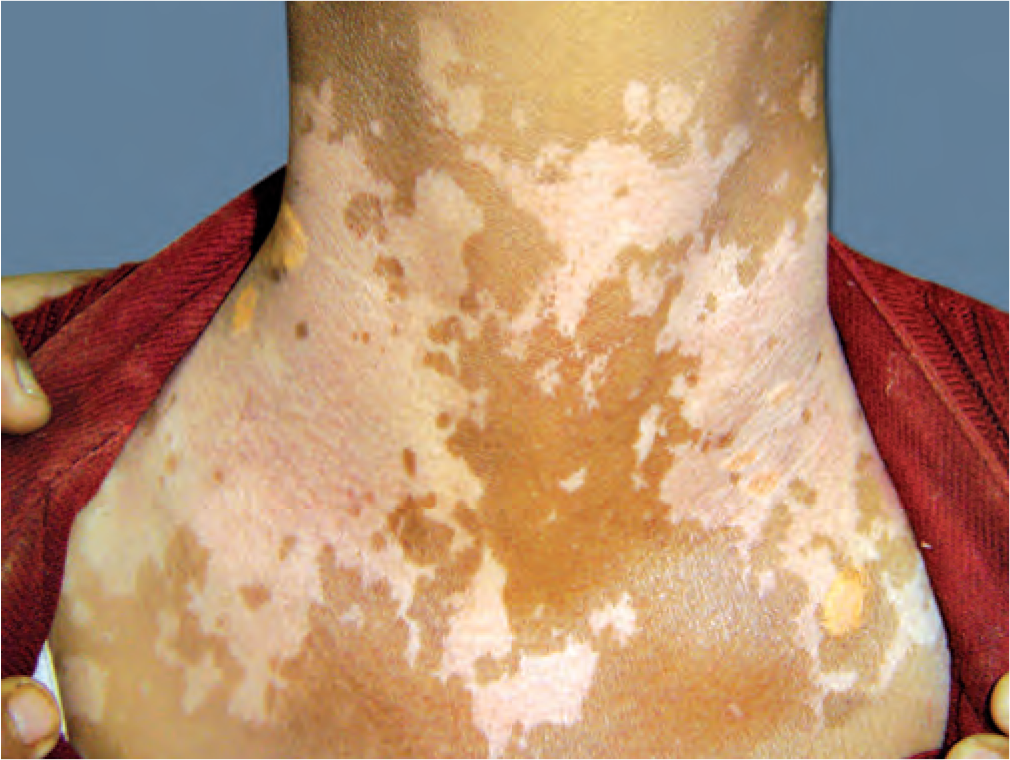
Medical treatments are not successful in all cases of vitiligo. Tissue grafts have the limitations that large amount of donor skin is needed as there is no cell expansion in these methods. Hence, transplantation of autologous cultured and noncultured melanocytes which involve cell suspension without culture or keratinocyte/melanocyte cocultures are gaining popularity. Transplantation of noncultured melanocytes/ keratinocytes suspension has the advantage that cell culture is not needed and that skin can all be undertaken in a single 3 hour procedure.
Procedure
- Harvesting a skin graft
- Trypsinization and cell separation
- Dermabrasion of the recipient (vitiligo) site
- Transfer and fixing of melanocyte rich cell suspension.
 Harvesting of Skin Graft
Harvesting of Skin Graft The lateral aspect of the gluteal region is selected as the donor area. Care should be taken to ensure that the donor area has no vitiligo patches. The area of the split thickness donor skin taken is one-tenth of the recipient area while dealing with large confluent patches. In cases, having multiple scattered small patches, larger donor skin is taken, approximately one-fifth of the recipient area. Under aseptic precautions, a very superficial sample is harvested using a shaving blade held in straight Kocher’s forceps. The donor area is dressed with liquid paraffin dressing (Fairlee™) and sterile gauze pad.
Cell Separation Technique
This is the most important step and consists of three steps; trypsinization, removal of excess trypsin by antitrypsin and centrifugation to obtain a cell suspension.
- Trypsinization: The cell separation is done ideally under aseptic precautions in a laminar flow bench kept in the operation theatre. If laminar flow bench is not available, the sterile environment of the theatre is adequate. The skin sample harvested is transferred to a Petri dish containing 5 ml of the 0.2% w/v trypsin solution, epidermal side facing upwards, and incubated for 45 min at 37°C.
- Removal of excess trypsin: After incubation for 45 minutes-2 hours, the action of trypsin is neutralized with trypsin inhibitor (Life Technologies, USA).The epidermis is separated from the dermis and transferred to a test tube containing 2 ml of DMEM: Nutrient mixture F-12 (DMEM/F-12) medium (Life Technologies) and vortex mixed for 15 seconds. The epidermis is further broken into smaller pieces in a Petri dish and washed with the DMEM/F-12 medium and finally transferred to a test tube containing the DMEM/F-12 medium.
- Centrifugation: The test tube is then centrifuged for 6 minutes. The supernatant is discarded and the pellet 361 at the bottom is suspended in a 1 ml insulin syringe.
The final volume prepared varied from 0.2–0.5 ml depending on the size of the graft taken and the area to be treated
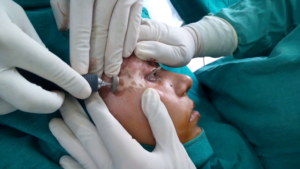 Dermabrasion of the Recipient Site
Dermabrasion of the Recipient Site
The recipient site is abraded with a dermabrader fitted with a diamond fraise wheel (Delasco™). While operating close to the eyelid margins, an erbium:YAG (Er:YAG) laser is used with a fluence of 1,000 mJ, 1–2 passes. The endpoint of ablation is pinpoint bleeding. Hemostasis is achieved and the ablated area is covered with saline-soaked gauze pieces.
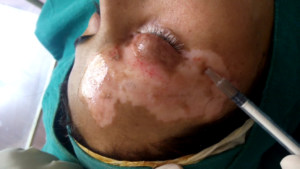
Transplantation Technique
The cell suspension is spread evenly on the dermabraded area through a pasteur pippette and covered with collagen dressing (Collomedica laboratories) to hold the cells applied. This is covered with liquid paraffin and gauze pieces. Patients are instructed to lie still in the same position for at least 1 hour to ensure cell fixation and then shifted to a room and further instructed to avoid excessive movements of the treated area for atleast six hours.
Postprocedure Instructions
All patients are instructed to take complete rest and avoid all vigorous physical activities. Patients are prescribed oral antibacterial agents for 5 days and nonsteroidal anti-inflammatory drugs (NSAIDs) for 3 days. The dressings are removed after 1 week in most cases. Patients are asked to follow up at weeks 1 and 3 and then at 3 month intervals. Patients are instructed not to scrub the area. Patients are permitted to use makeup on the treated area 10 days after the removal of dressings.
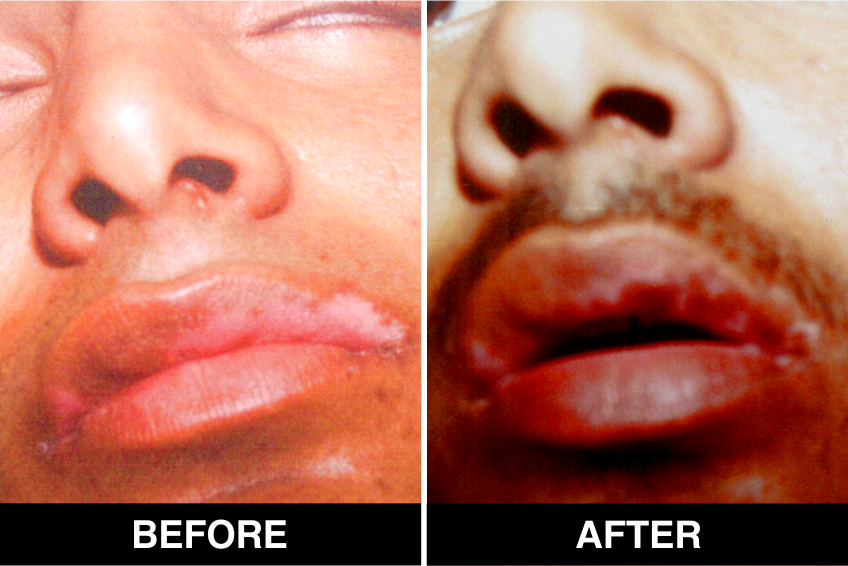
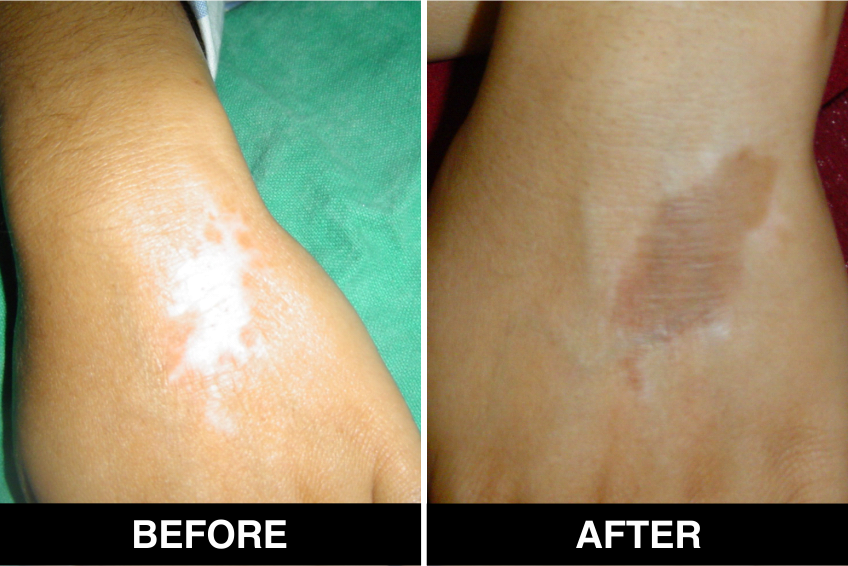
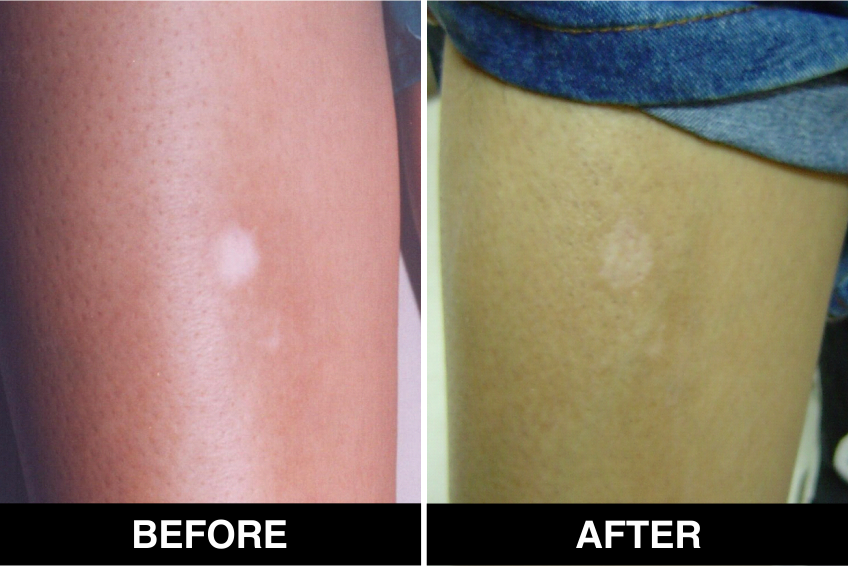
Onset of Pigmentation
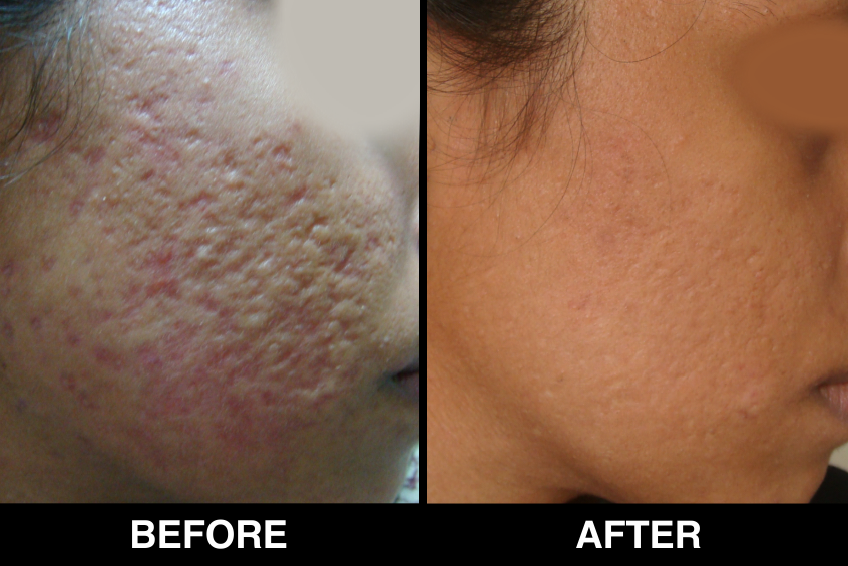
The onset of pigmentation usually occurs in 3–6 weeks and it can take 3–6 months for the patches to achieve significant pigmentation. Psoralen ultraviolet A (PUVA) with sunlight or phototherapy can be initiated after 3 weeks. Vitiligo patches which don’t recover even after 6 months will need to be transplanted again.
Advantages of Melanocyte Cell Transplantation
- Donor recipient ratio 1:10 i.e. with just 10 cm2 of donor size a vitiligo patch of 100 cm2 can be treated
- Excellent texture and color matching
- No stuck on look (as seen in split thickness grafting) or cobblestoning (as in punch grafting)
- Large areas can be treated in single session
- Patient can use cosmetic camouflage as early as 10 days postoperatively
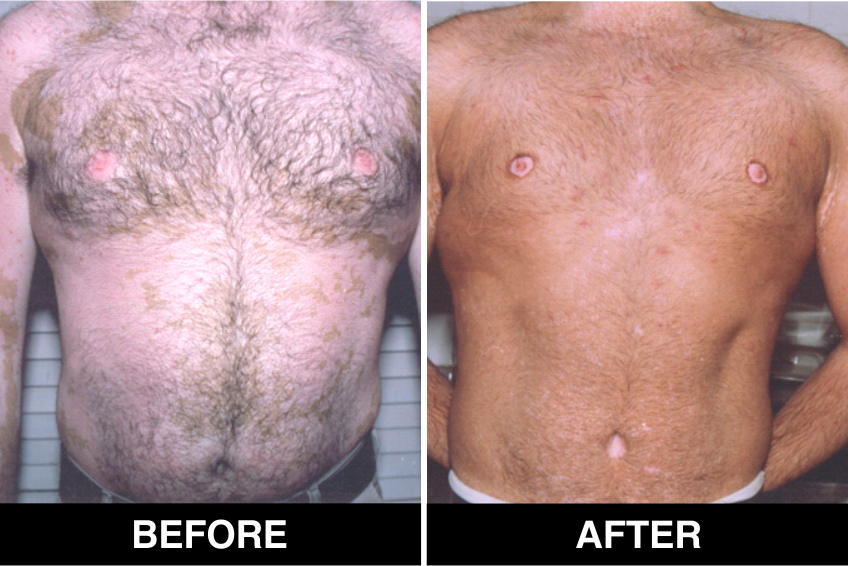
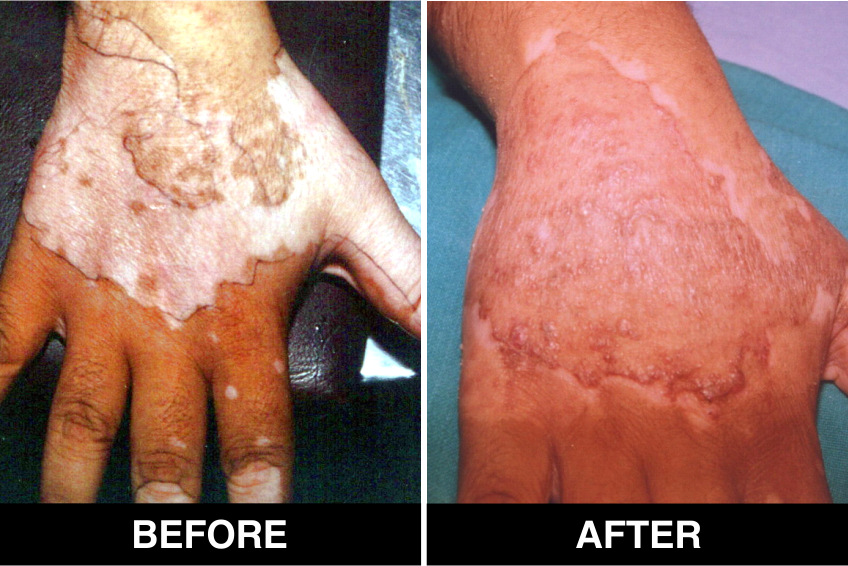
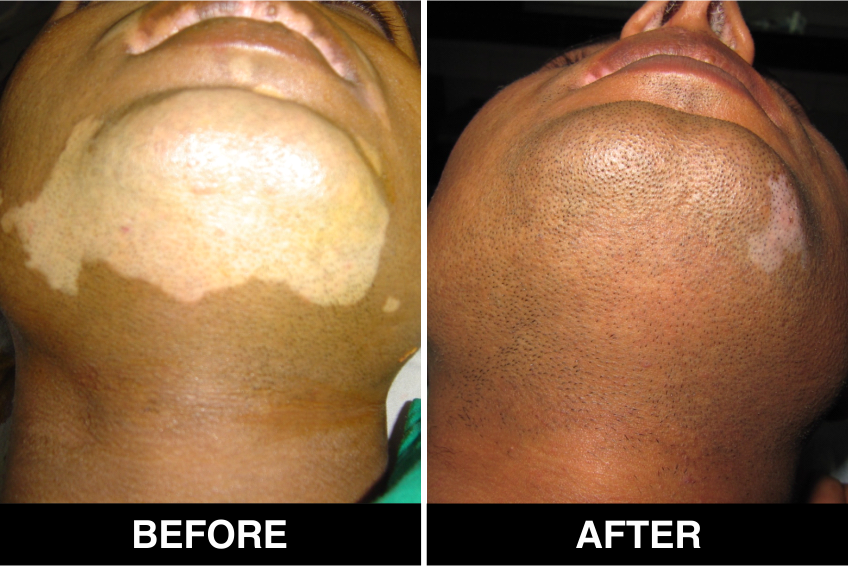
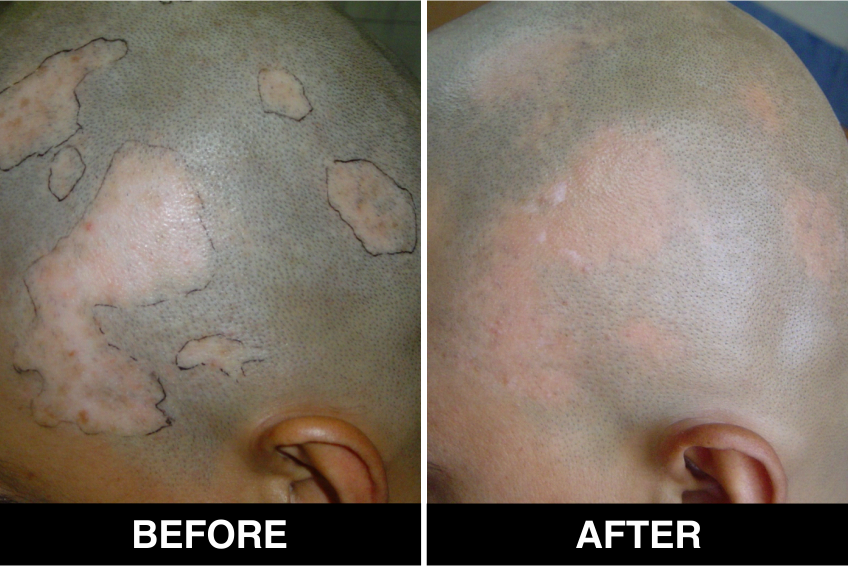
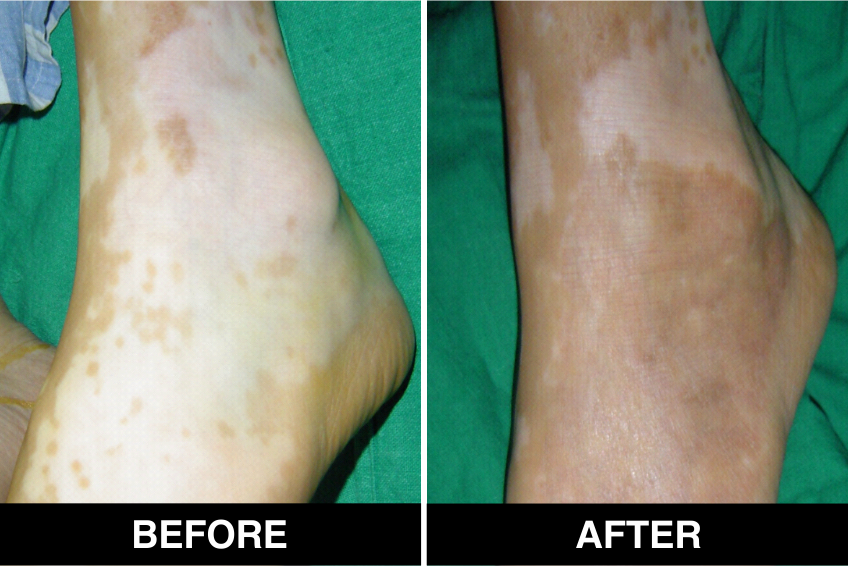
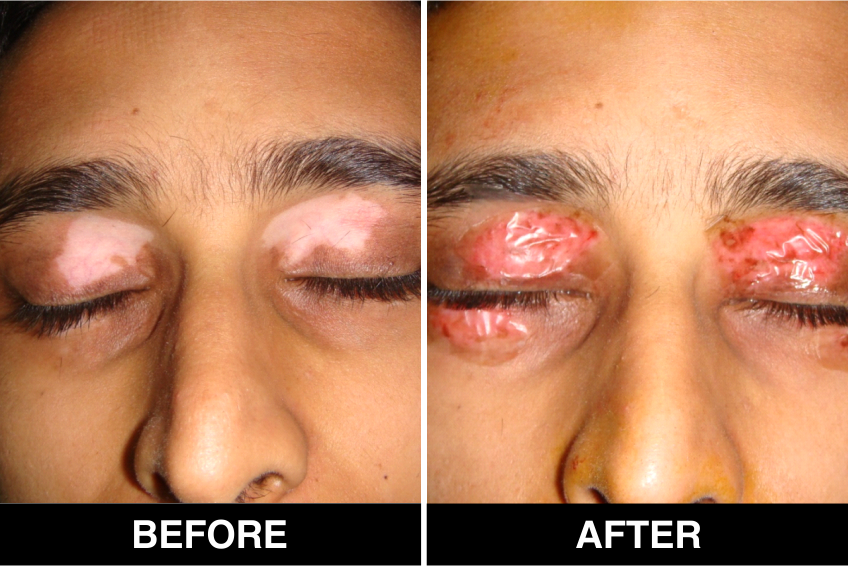
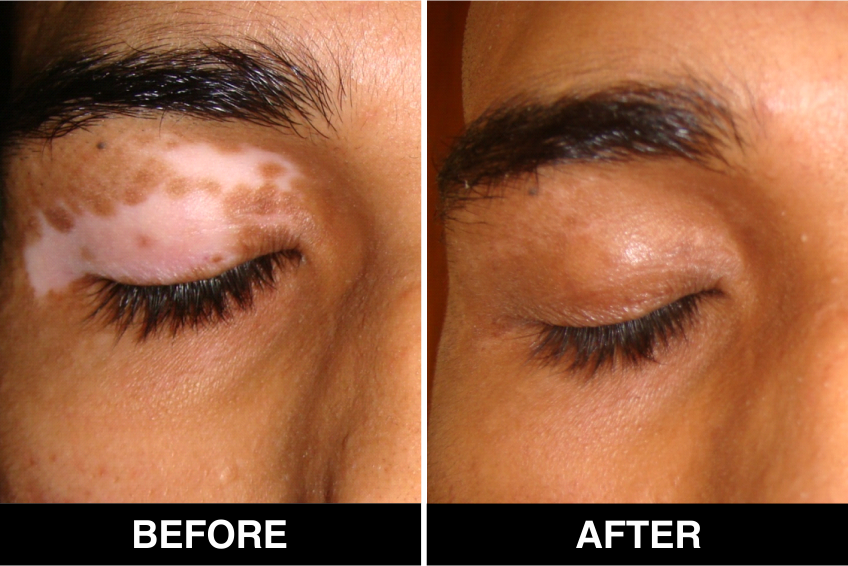
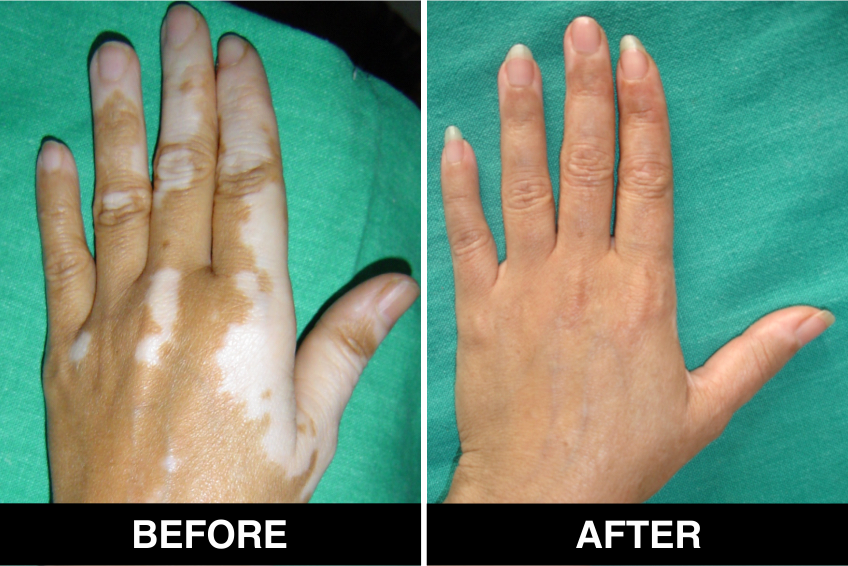
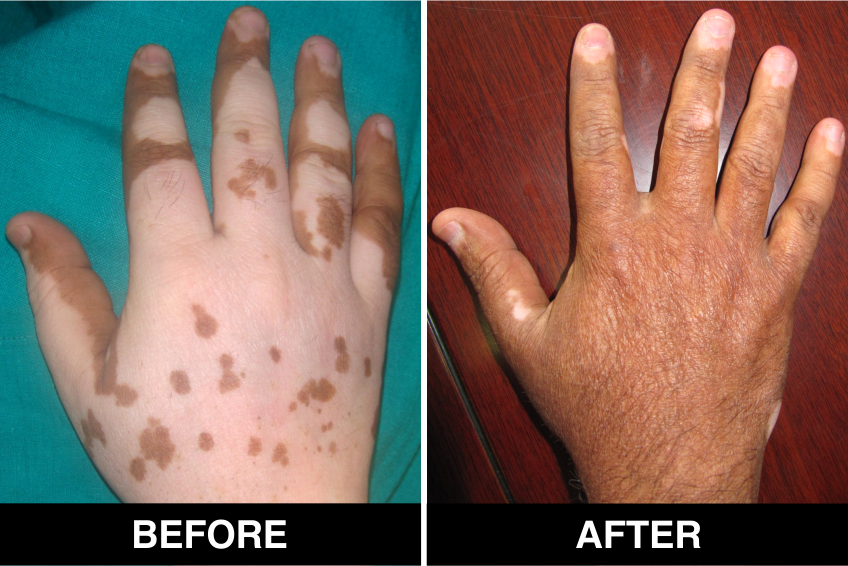
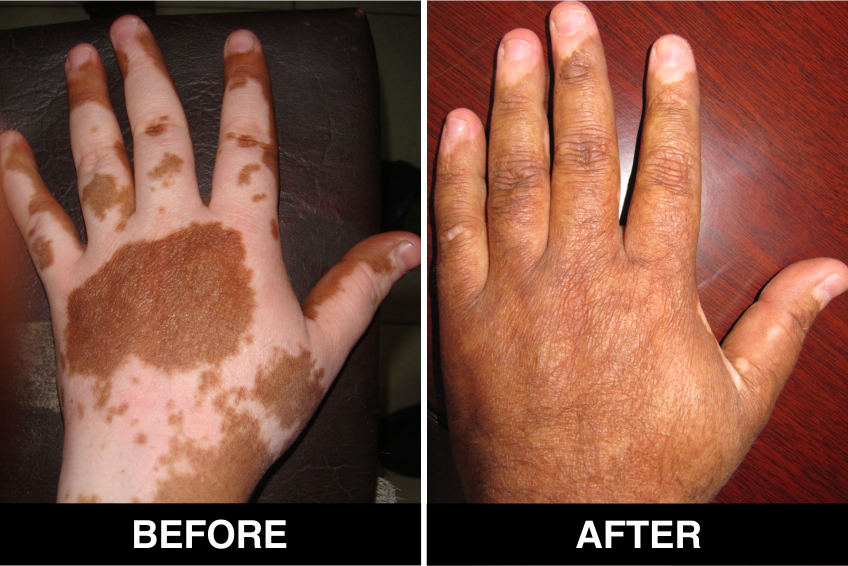
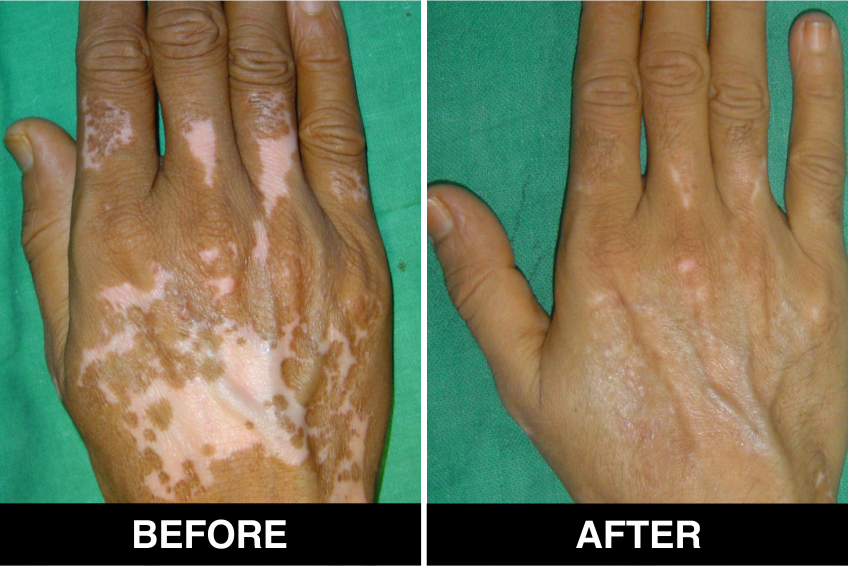
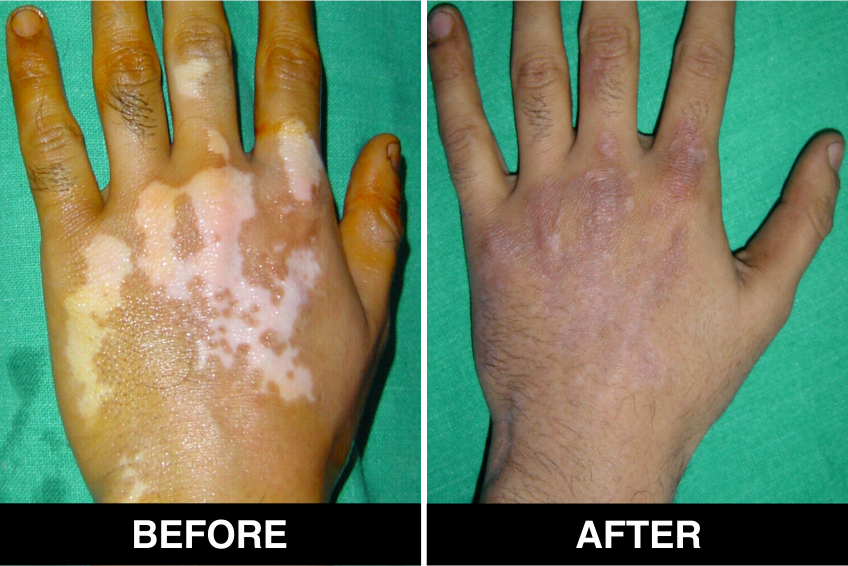
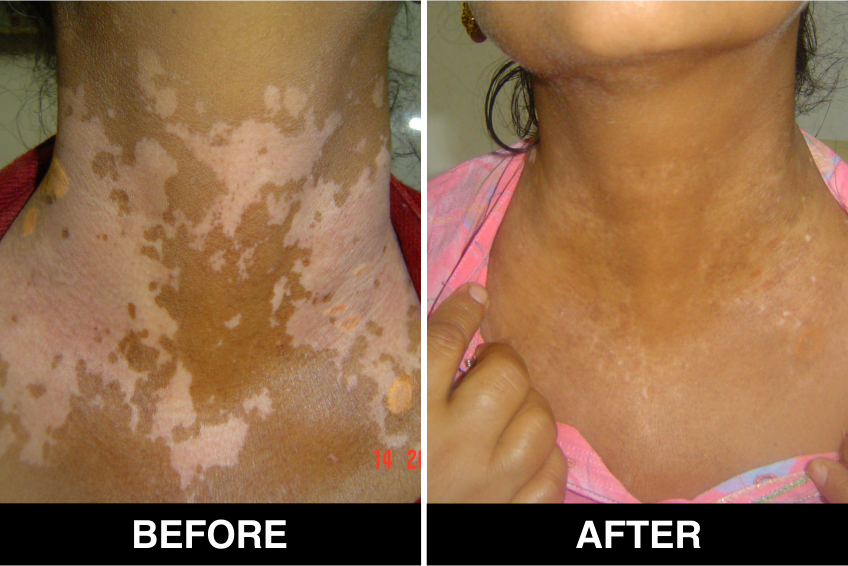
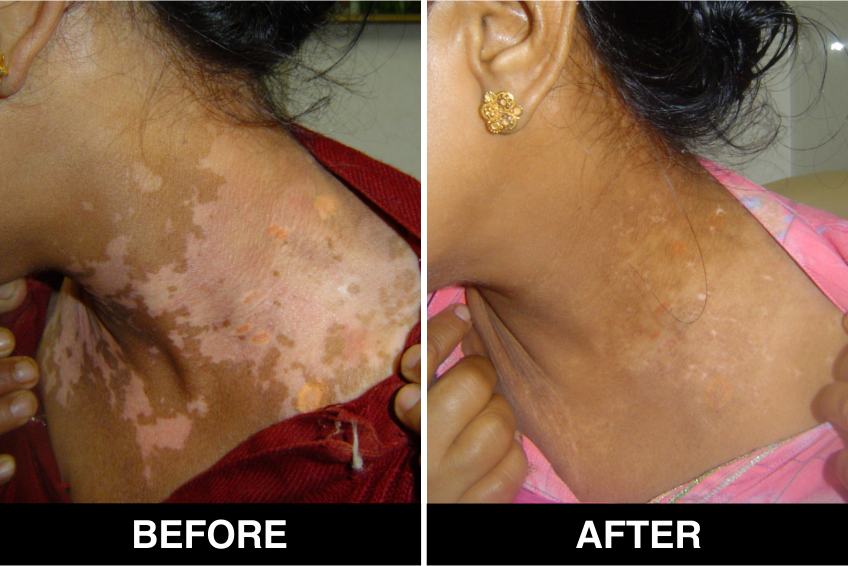
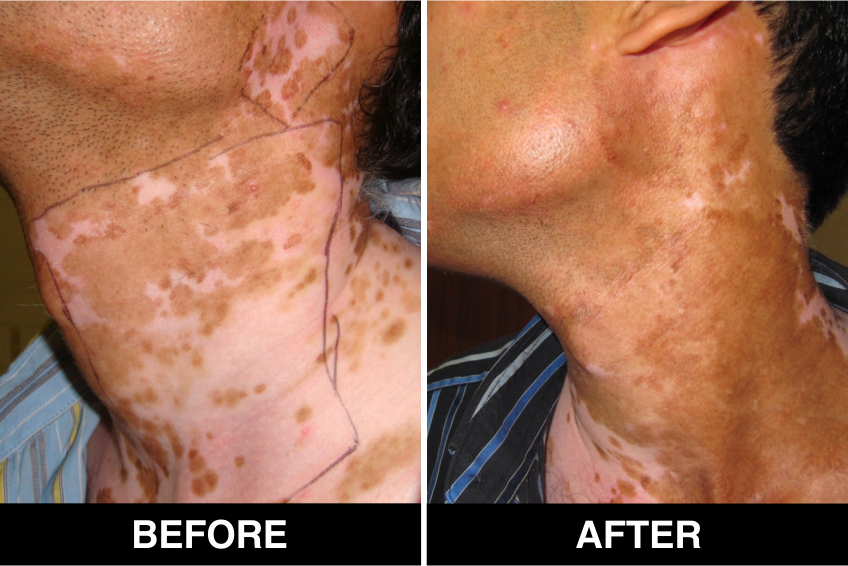
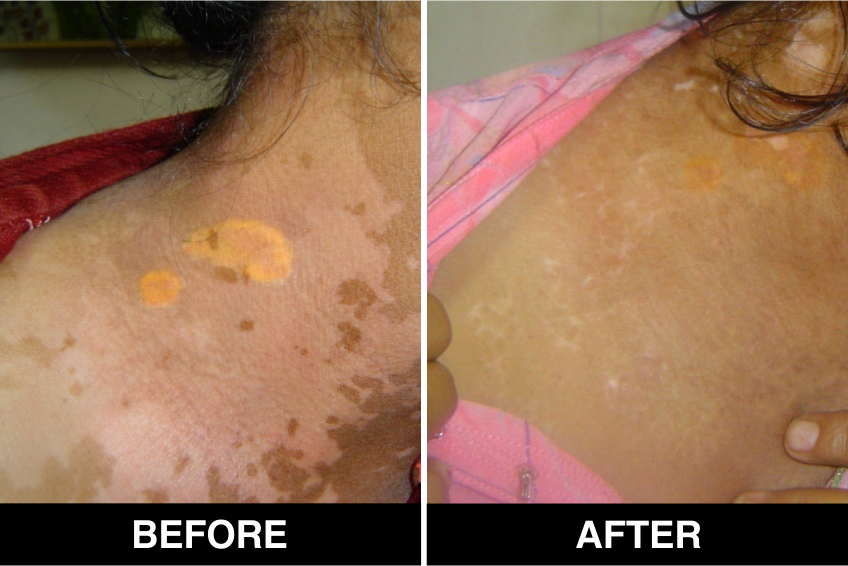
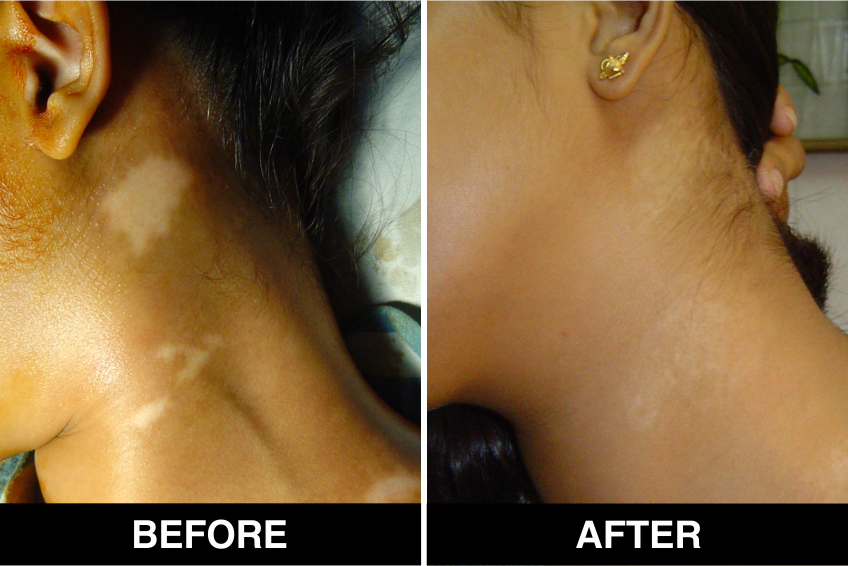
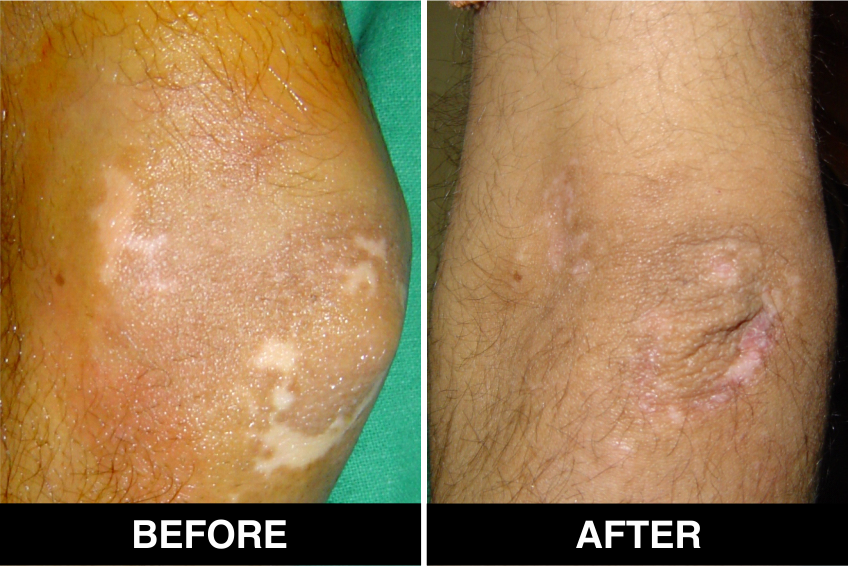
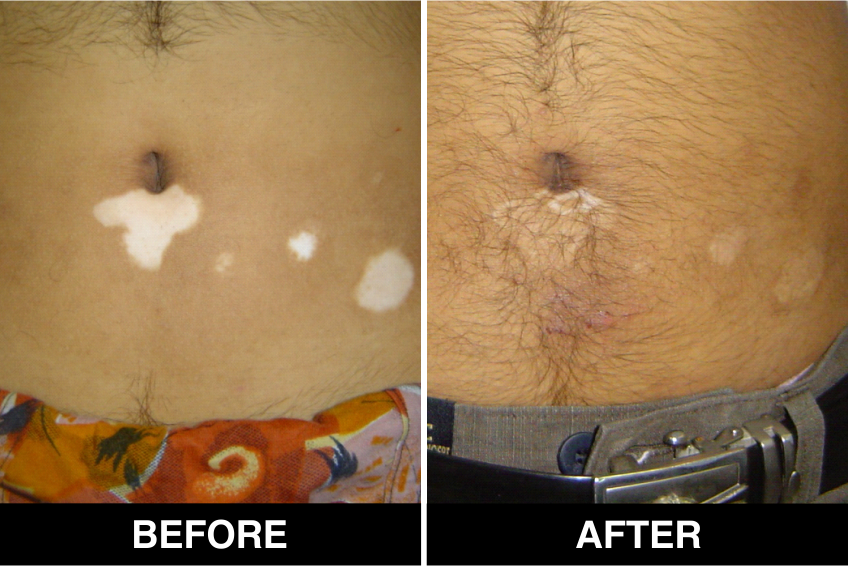
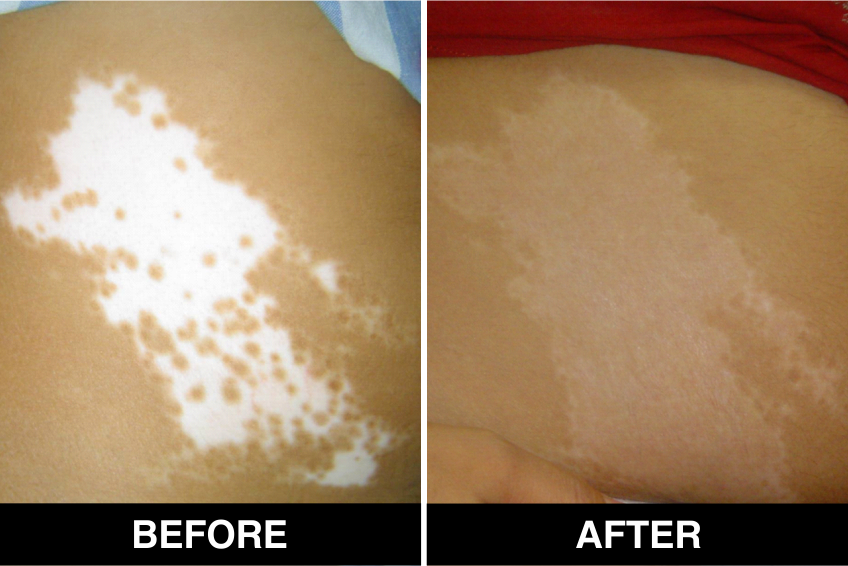
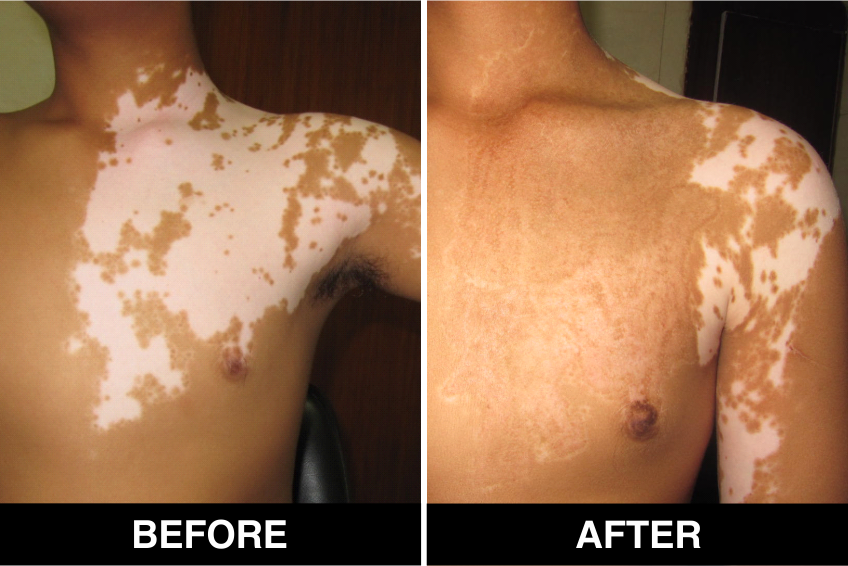
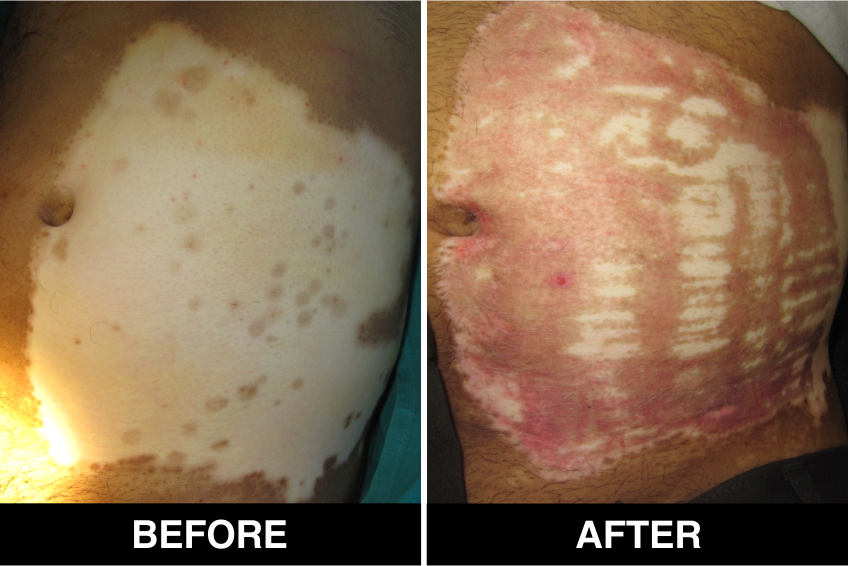
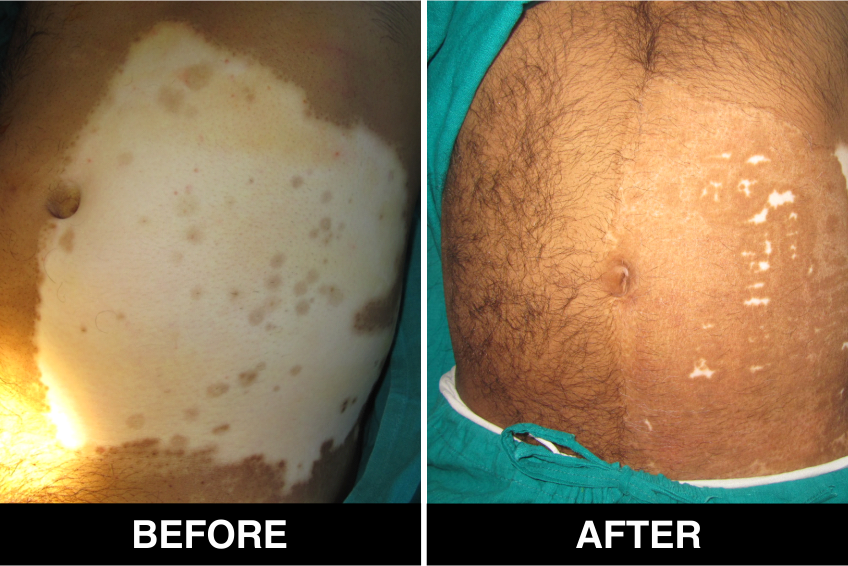
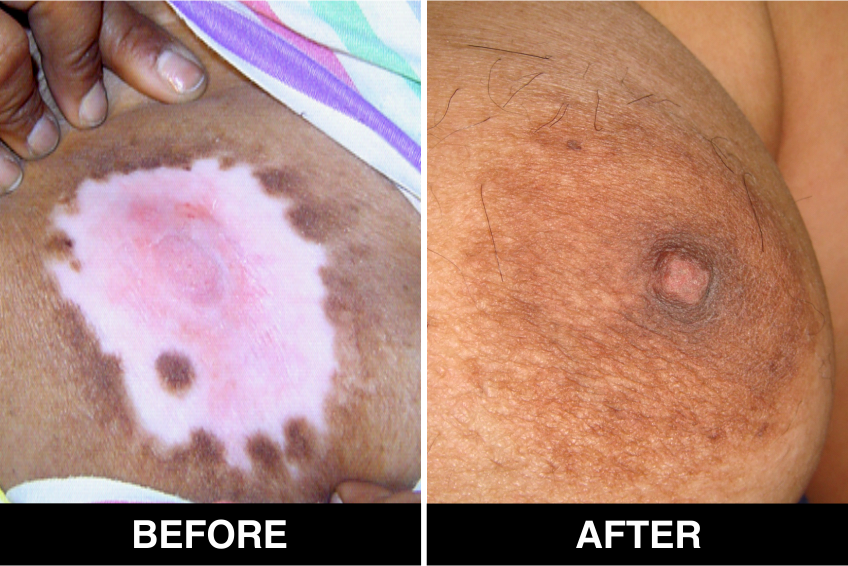
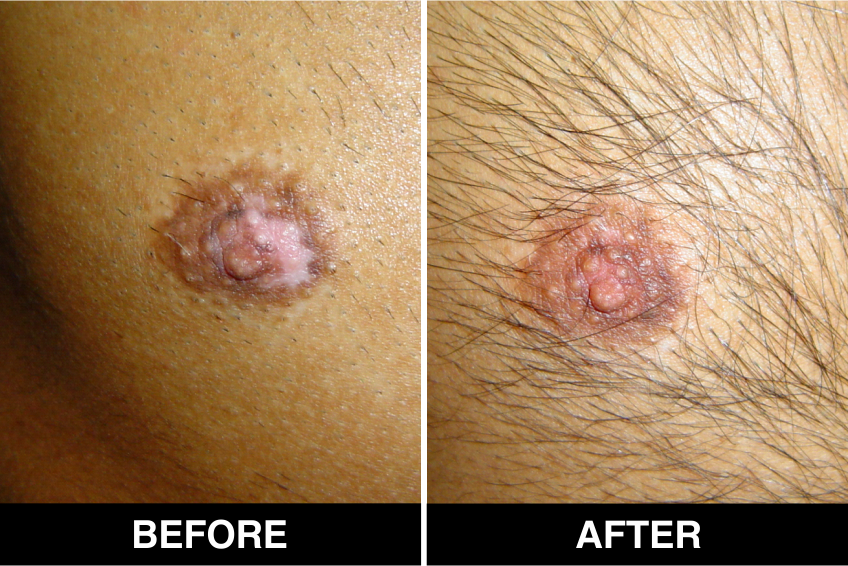
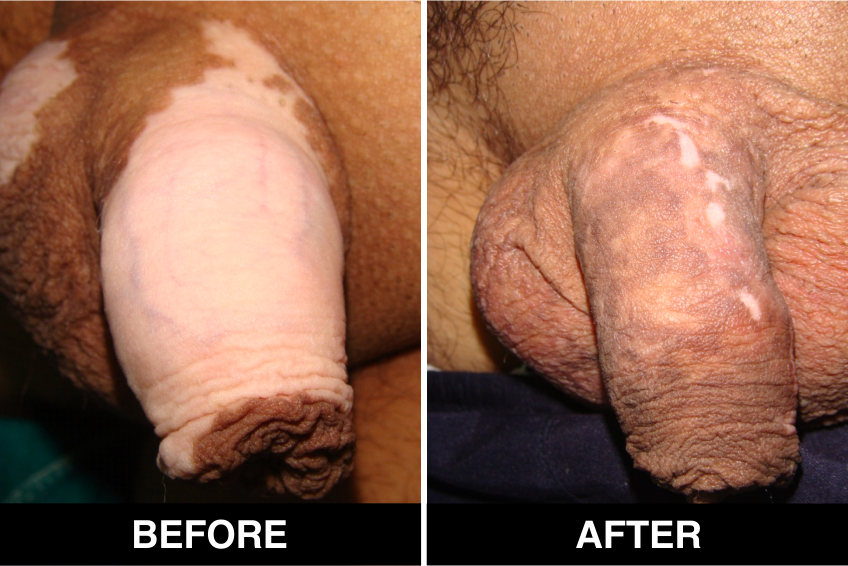
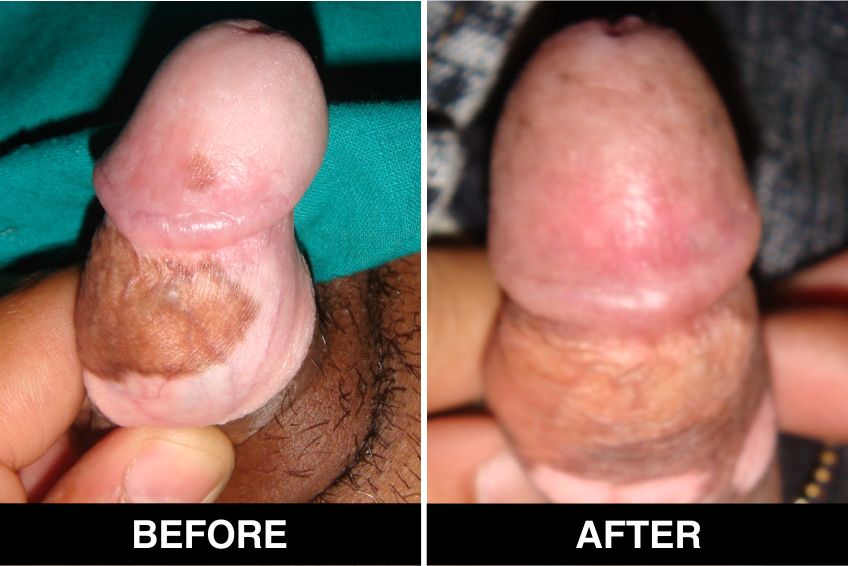
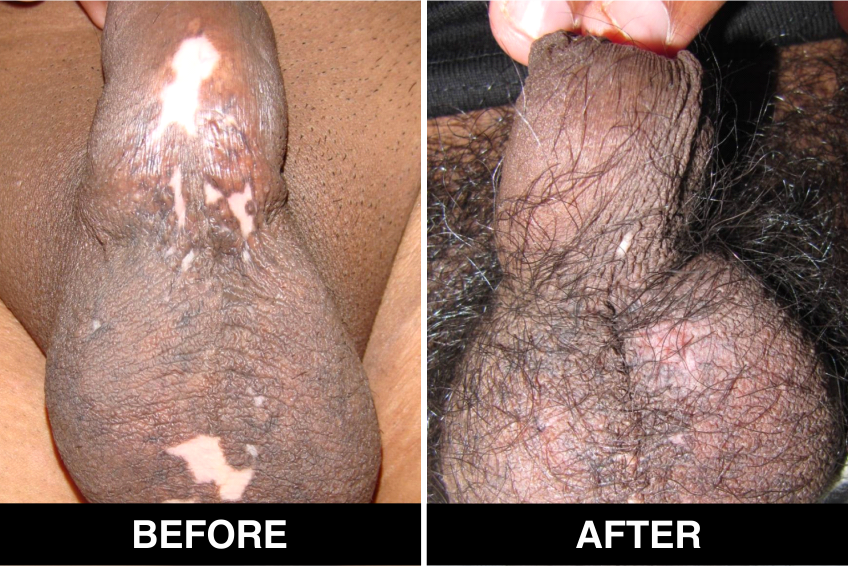
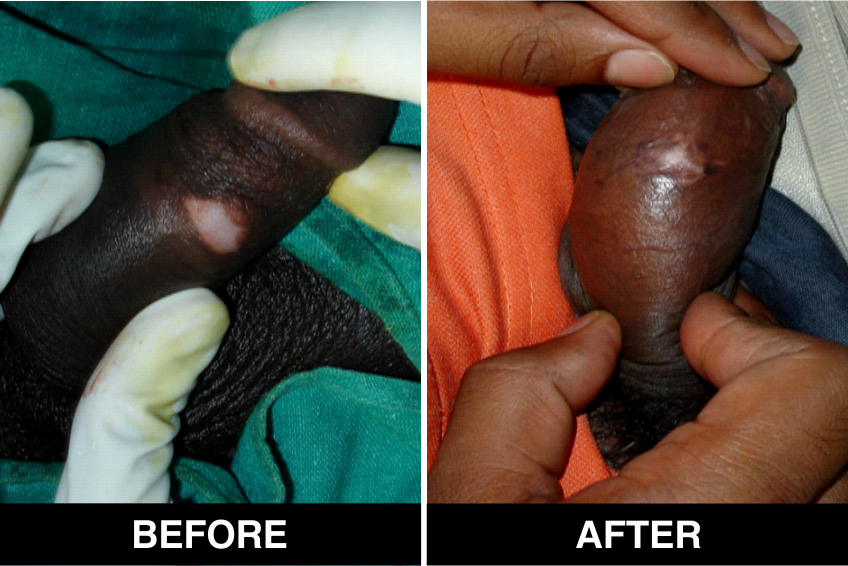
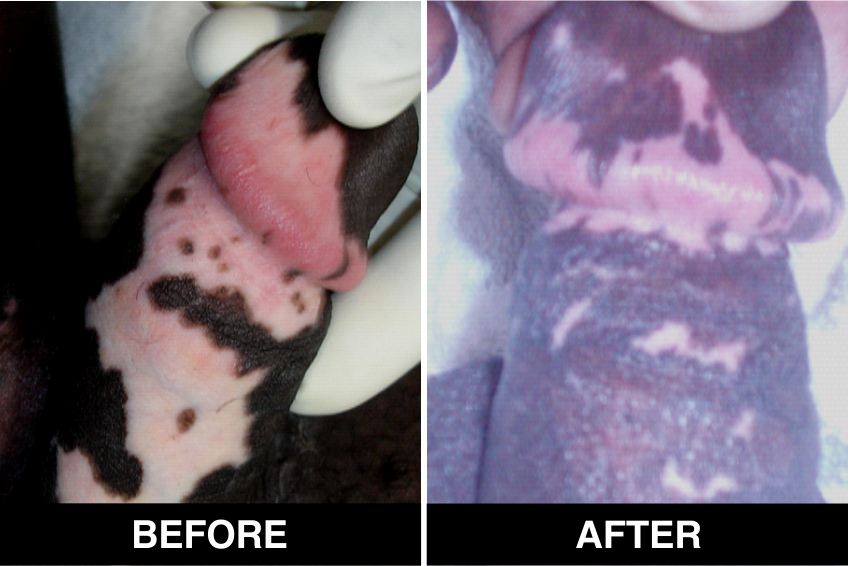
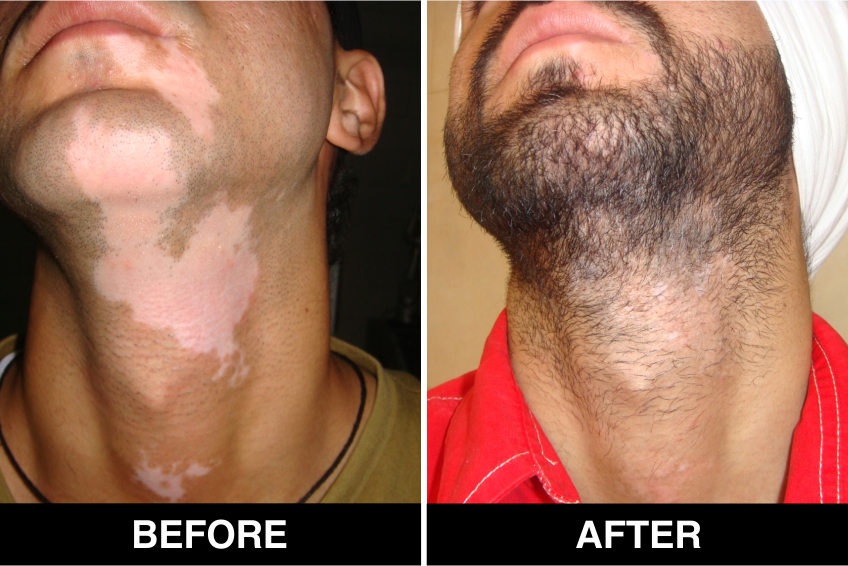
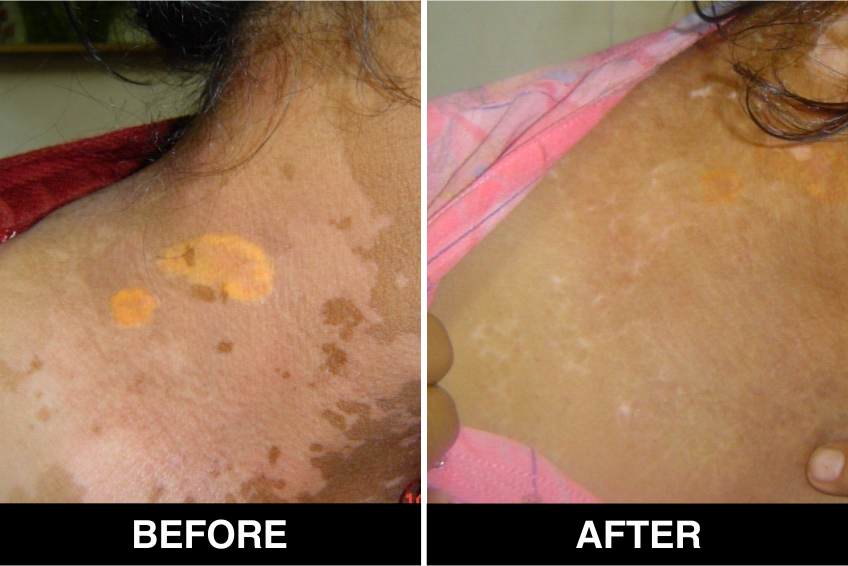
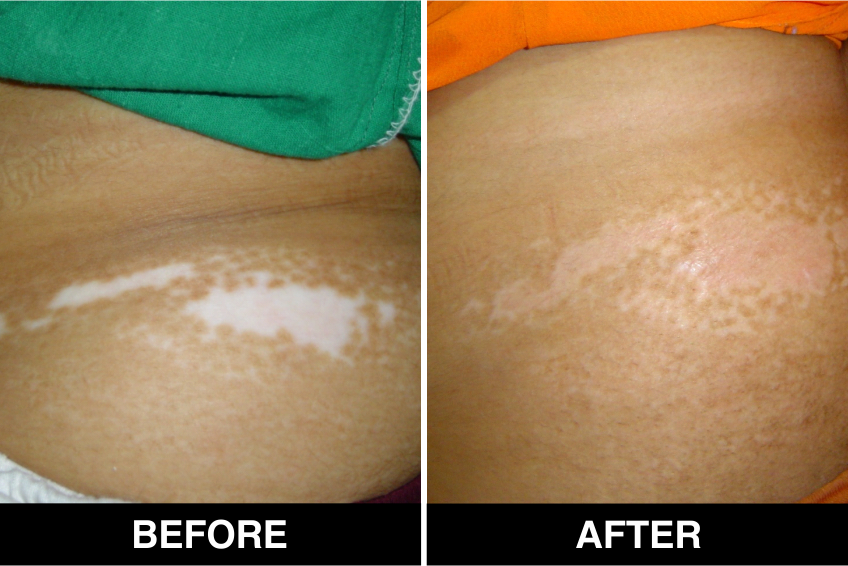
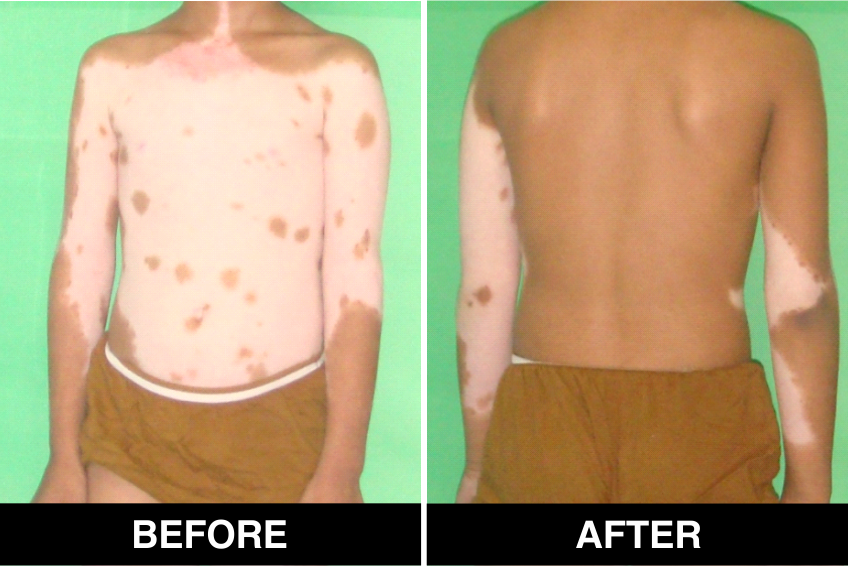
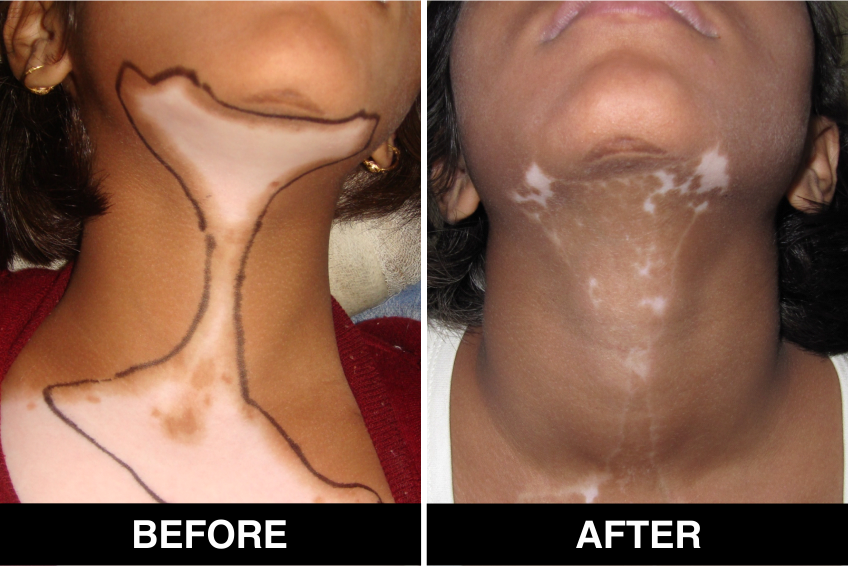
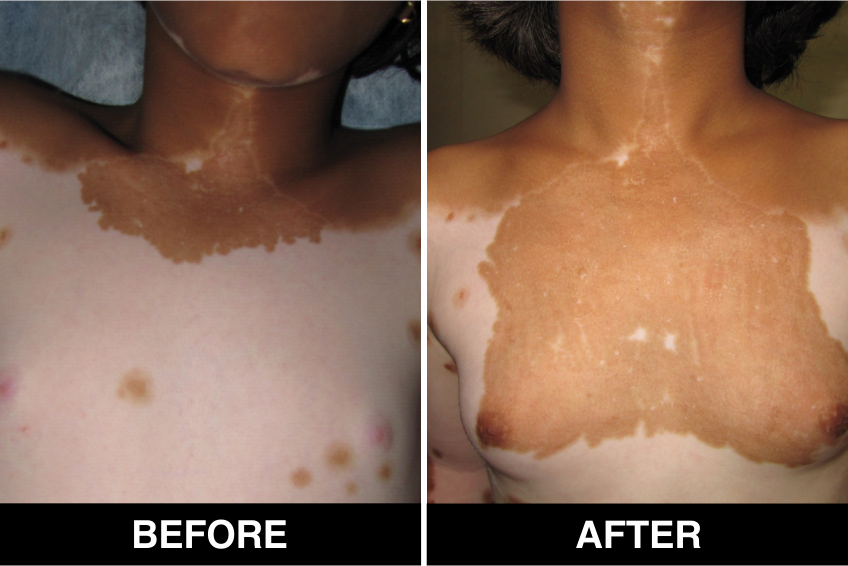
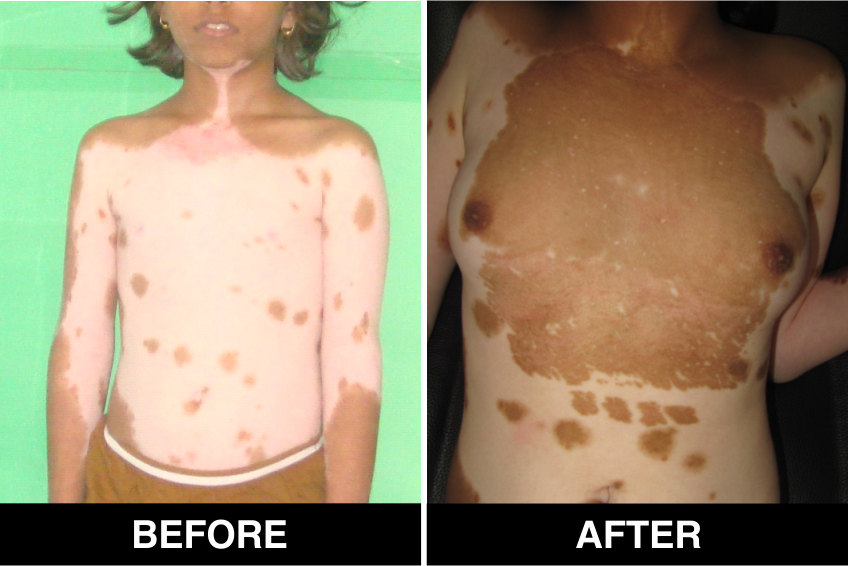
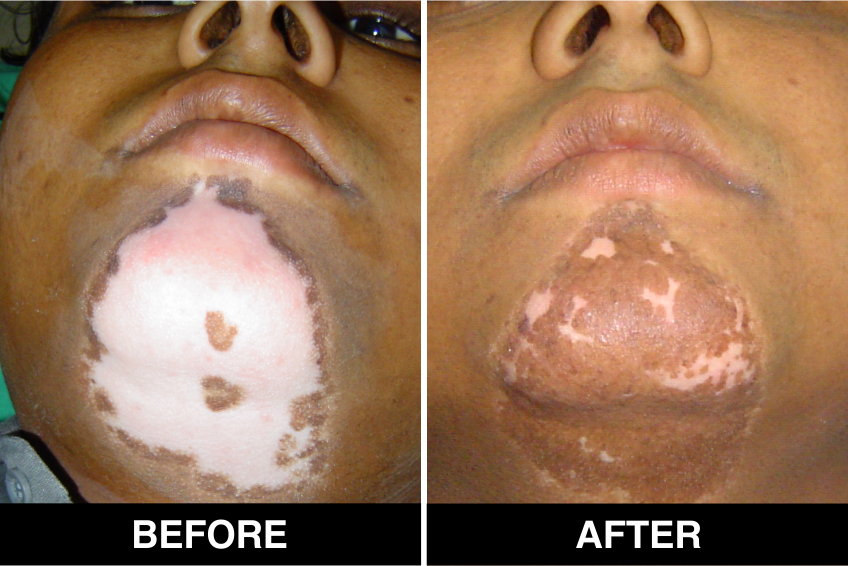
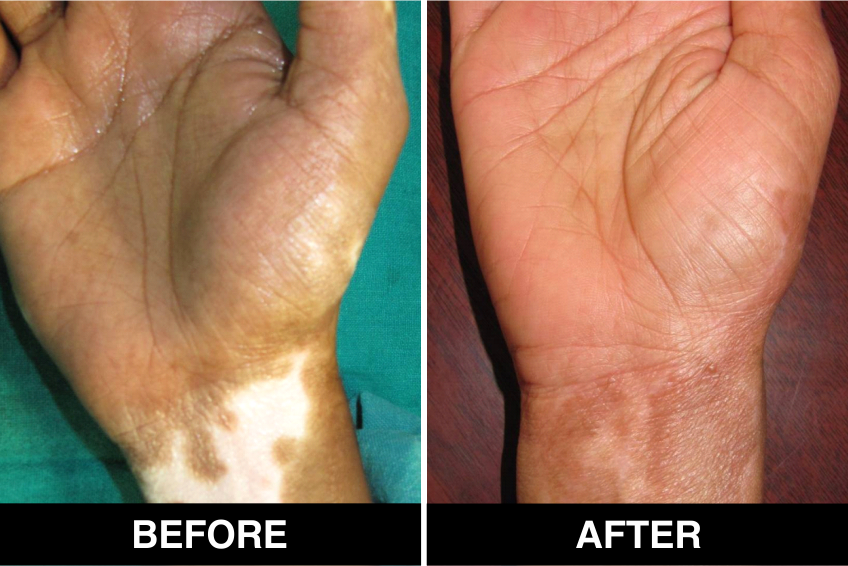
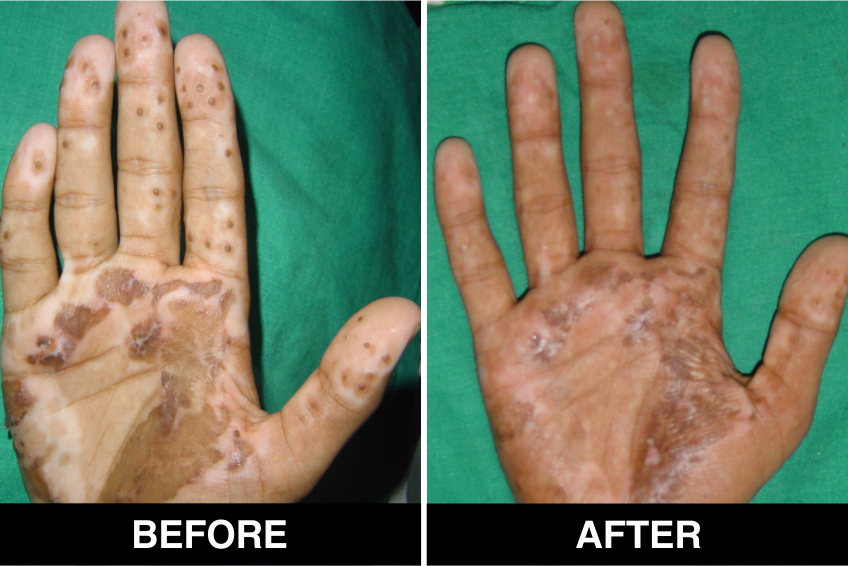
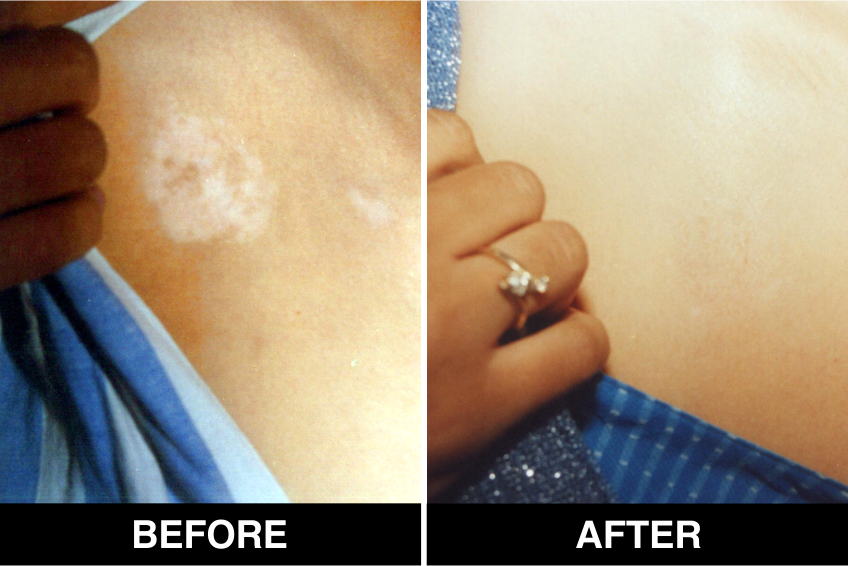
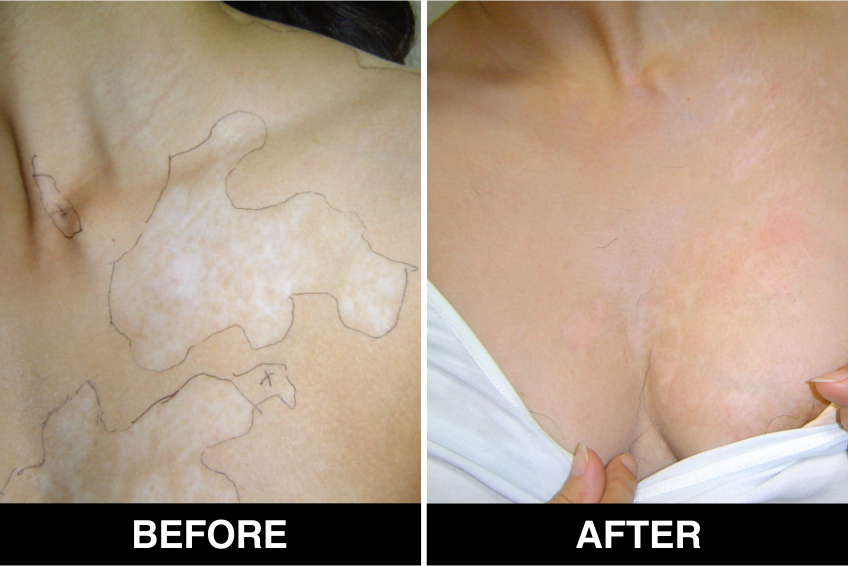
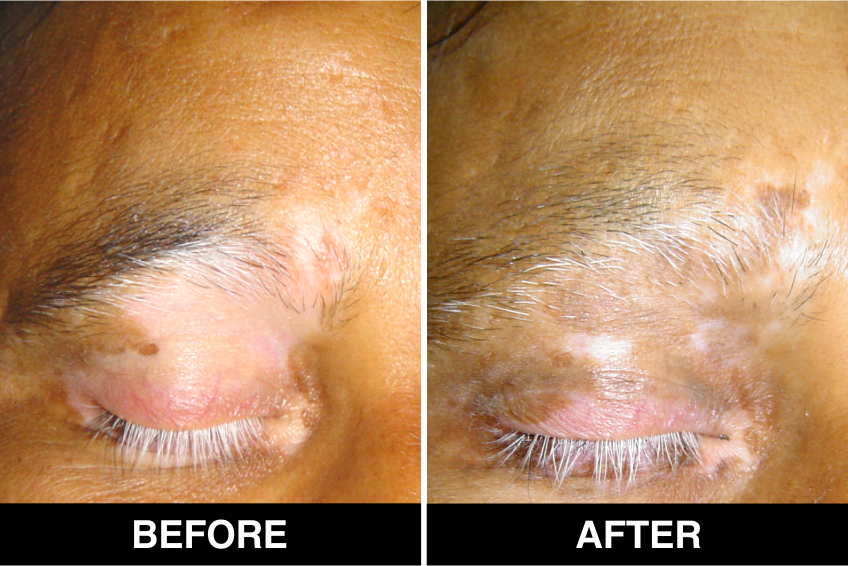
Melanocyte Treatment FAQ’s
It takes around 2-3 hours for the procedure to be performed.
Advantages of Melanocyte Transplantation
1. It is a day care procedure. Patient can go home in 3 to 5 hours.
2. A large area can be treated in one operative session.
3. A very small piece of normal skin is sufficient to treat large affected area, e.g. 10cm2 of donor skin is enough to treat 100 cm2 of vitligo / leucoderma patches.
4. Very good cosmetic results.
5. Repigmentation is seen in 2 months and may take 4 to 6 months for maximum improvement and proper color matching.
6. Very minimal or no side effects.
7. No postoperative phototherapy required.
Sometimes a few white spots remain. Approximately 30% patients require repeat grafting for complete recovery.
In one operative session 100 to 500 cm2 can be treated, small areas can be done under local anesthesia, Large areas ( Gega or Mega Sessions Areas>150 cm2 would require General Anesthesia
The treated site is dressed for one week. Verbal and written post treatment instructions are provided. Upon removal of dressing, the treated area appears red. Re-pigmentation begins in 4 to 8 weeks and continues to progress up to 3 to 6 months post-grafting.
Book An Appointment